Blue Waffle Disease: STI Hoax or Facts
What is blue waffle disease?
Stories of the blue waffle disease began circulating around 2010. The blue waffle disease emerged when an image speculated to have been a graphic image of a sexually transmitted infection (STI) was seen online. The image was of a labia tinted blue, covered with pus, and filled with lesions discovered on the internet. The blue waffle disease is just a hoax with no medical proof.
This article looks to demystify the hoax called blue waffle disease and how real STIs are gotten.
The Hoax Called Blue Waffle Disease
The hoax called blue waffle disease began when internet pranksters posted an image of a supposed blue-colored vagina as a bait-and-switch meme. Waffle is a slang term used for the vagina. Hence the term “blue waffle” was coined to describe a serious vaginal infection. The blue waffle disease is said to be an STI. While some individuals claim that only persons with vaginas can develop this disease, others claim that only females with multiple sexual partners can get the disease. There are also claims that women who do not practice good hygiene can get blue waffle disease.
Symptoms of Blue Waffle Disease
Symptoms that were rumored to be associated with the blue waffle disease are bruises, a smelly discharge, lesions, and blue coloration. Other symptoms claimed to be associated with blue waffle disease are similar to symptoms of vaginal infection and real STIs such as chlamydia and gonorrhea. Medically, the blue waffle disease is a myth, but various STIs occur in sexually active individuals infected with a viral or bacterial infection. Some STIs have symptoms such as lesions and bruises but certainly not the blue coloration.
Sexually Transmitted Infections (STIs)
Sexually active people have an increased risk of contracting several existing STIs. Such individuals should monitor their genitals and visit a medical doctor if they observe something unusual. The signs and symptoms of some common STIs are seen below.
Gonorrhea
Caused by the bacterium called Neisseria gonorrhoeae, gonorrhea is an STI that targets warm and moist areas in the body such as the eyes, vagina, anus, female reproductive tract, throat, etc. It affects both males and females who are sexually active, but it is common in individuals between the ages of 15 and 24. If left untreated, it can cause complications as serious as infertility.
Generally, gonorrhea is asymptomatic, but it may cause symptoms that vary in both genders. The symptoms also depend on the location of the infection.
Symptoms in the vaginal or penis include:
- pains or burning sensation when urinating,
- inflammation in the testicles,
- increased discharge from the vagina,
- bleeding between periods,
- pains in the lower abdominal region,
- pains during sex,
- green, white, or yellow discharge from the penis.
Symptoms noticed when the rectum is infected include:
- rectal discharge,
- pains,
- rectal bleeding,
- pains in the bowels,
- anal itching.
Bacterial Vaginosis (BV)
Bacterial vaginosis is a vaginal infection caused by an imbalance or overgrowth of beneficial and harmful bacteria in the vagina. It is common among women of ages 15 to 44 years in their reproductive years. The risk of developing BV increases when the vaginal pH is altered by activities such as engaging in sex with multiple partners, douching, etc. It is still unclear why women develop it.
It is usually asymptomatic, but when it is symptomatic, the symptoms include;
- a fishy smell,
- white or grayish vaginal discharge,
- itchy or burning sensation in the vagina.
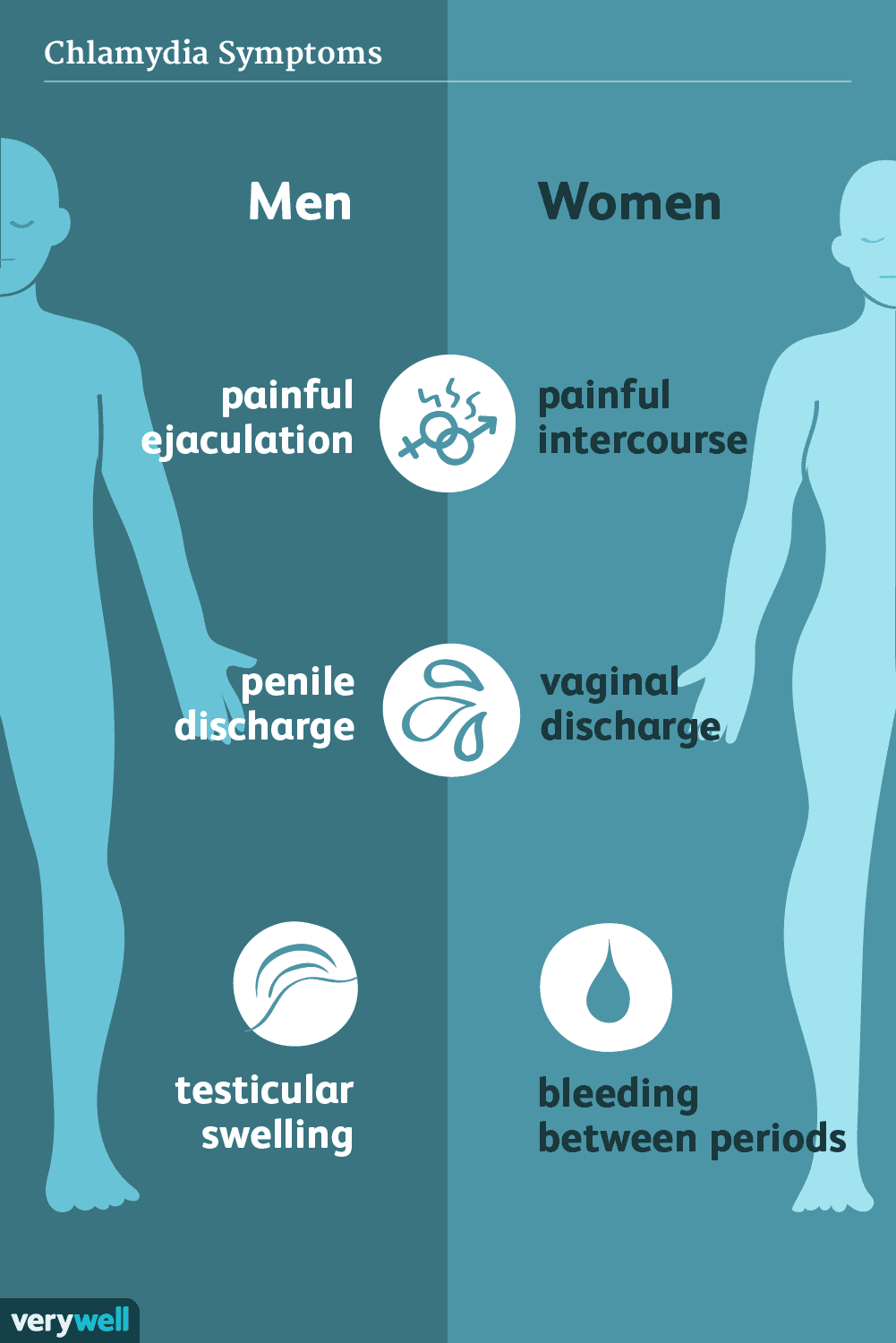
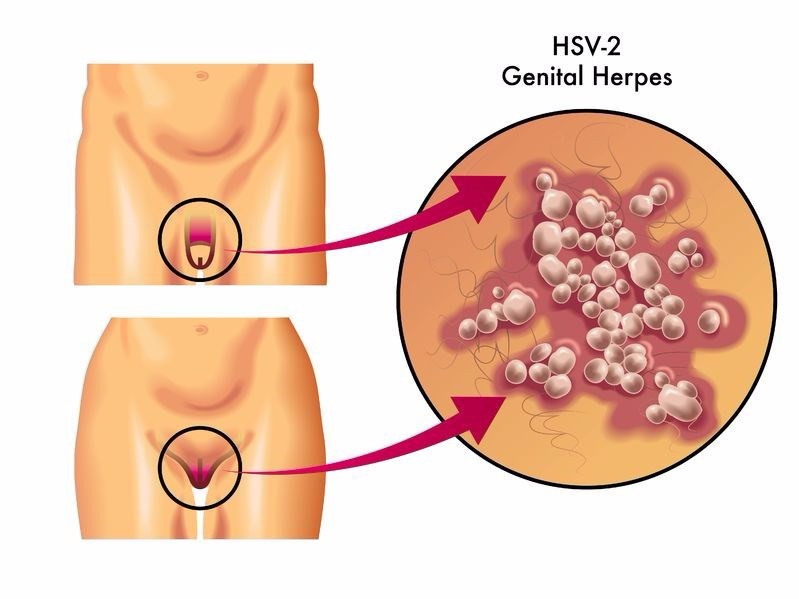
Chlamydia
Chlamydia is an STI spread via vaginal discharge or semen during sexual contact. It can affect just about anyone regardless of age, but it is most common among women. If not properly treated or not treated on time, it can lead to complications affecting a woman’s fertility. It is mostly asymptomatic, like bacterial vaginosis, but if symptoms develop, it can take a couple of weeks before it is noticed. Symptoms experienced include:
- an unusual discharge from the vagina,
- discharge from the penis,
- inflammation in one or both testicles,
- burning sensation during urination.
- painful urination
- testicular swelling
- bleeding between periods
When transmitted via anal sex or the rectum is affected, symptoms experienced include;
- bleeding in the rectum,
- pains in the rectum,
- discharge from the rectum.
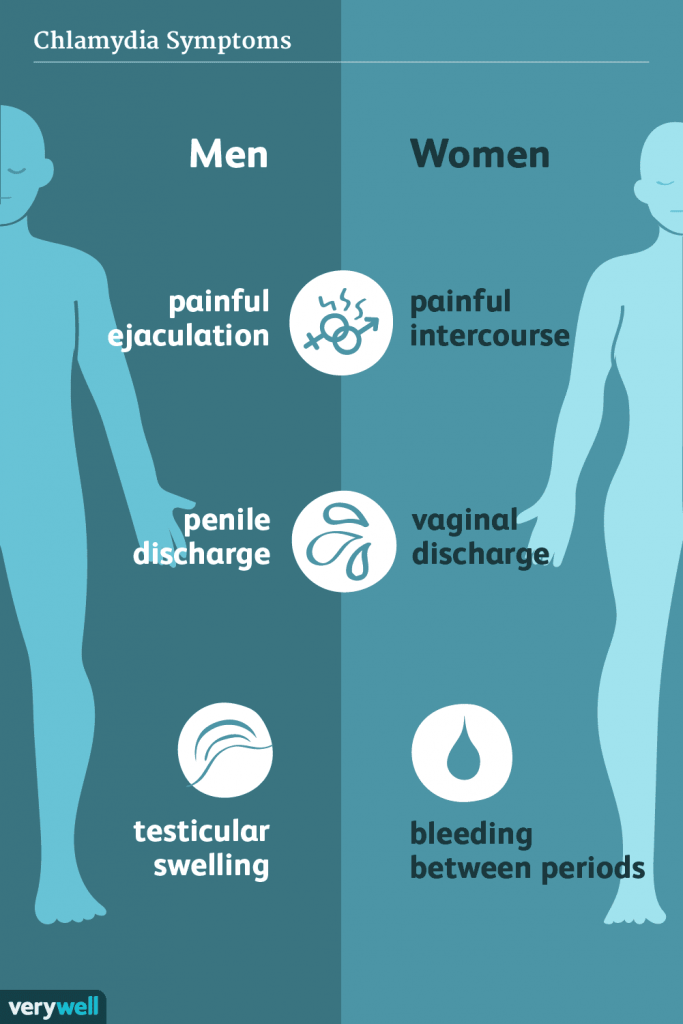
Genital Herpes
The herpes simplex virus, associated with pains and sores in the genitals, causes genital herpes. The herpes simplex virus is of two types, the HSV-1 and HSV-2. They can cause genital herpes, but HSV-2 is known to cause genital herpes more. It is majorly spread through sexual contact. It affects males and females equally. Herpetic sores are formed, which result in fluid-filled painful blisters that can ooze out fluid when they break open.
Genital herpes has no cure, and once an individual is infected with the virus, it stays dormant in the body. The virus, however, can be reactivated after some time. Symptoms start showing between day 2 to day 12. Most people exposed to the virus are either asymptomatic or experience mild symptoms.
Symptoms include:
- fever,
- body aches,
- headaches,
- long-lasting lesions,
- swollen lymph nodes,
- viral shedding increases (at this point, the virus can easily be transmitted).
After the first outbreak of herpes symptoms has been resolved, the symptoms can still occur from time to time. The symptoms become less serious, and they do not stay long. Prodromal symptoms are symptoms that occur during recurrent outbreaks of the virus. Such symptoms include genital pains and pains in the lower part of the body. They serve as a harbinger of a herpes outbreak.
Human Papillomavirus (HPV)
According to the Centers for Disease Control and Prevention (CDC), this is the most common STI caused by a virus that can be transmitted via skin contact. It has been reported that there are over 200 varieties of HPV, out of which 40 of these varieties of HPV are spread through sexual contact. It affects the mouth, throat, or genitals. While not all types of genital HPV may result in medical issues, some types can result in health problems such as genital warts, and some others can result in cancer of the anus, cervix, penis, vagina, vulva, oropharyngeal, and throat. Generally, many infections caused by HPV are asymptomatic and do not require treatment. However, once an individual has been infected by HPV, the virus stays in the body but is dormant rather than active. It can also be spread via sexual contact in its dormant state.
Testing for Sexually Transmitted Infections
Many people living with STIs have not yet been diagnosed, mostly due to the non-present symptoms of STIs. As a result of stigmatization, people living with STIs are not courageous enough to get treated. If left untreated, the STI can lead to serious health problems such as cancer, infertility, etc.
As long as an individual is sexually active, going for STI testing is important, especially in cases when:
- the individual engages in sexual intercourse with many partners,
- experiences symptoms indicating the presence of an STI,
- engaging in sexual intercourse with a new partner, etc.
One should seek help from a healthcare professional when there is any indication of infection. It is important to be tested for STIs such as syphilis, gonorrhea, hepatitis B, HPV, HIV, chlamydia, etc.
Before an STI test is conducted, it is important to inform the doctor about:
- type of contraception used,
- medications taken,
- potential exposure to an STI,
- number of sexual partners,
- pregnancy status, etc.
The individual to be tested should also inform the healthcare practitioner if they have ever engaged in anal sex. STIs transmitted via anal sex can not be detected in standard STI tests. One can do the test in hospitals, some pharmacies, and healthcare clinics funded by the government.
The tests may require;
- the use of swabs to collect cells from any part of the reproductive system,
- Collecting samples of an individual’s blood or urine to run tests for STIs such as chlamydia, gonorrhea, syphilis, and HIV,
- Conducting a physical examination around an individual’s genitals and anus for herpes and genital warts.
Blue waffle disease is not a real disease, but individuals are advised to practice good hygiene. It is also advised to go for STI testing and be vigilant for changes in the genitals and the reproductive part of the body.
FAQ
1. What is a blue waffle disease?
Blue waffle disease is a non-existent sexually transmitted infection (STI). A false story about blue waffle disease was spread through the internet, claiming that it gives the vagina a blue coloration.
2. What are the causes of blue waffle disease?
The causes are unknown because blue waffle disease is a hoax
3. Does blue waffle disease affect only females?
Blue waffle disease does not affect both females and males. It is a completely fictional story with no medical backing.
4. How can blue waffle disease be transmitted?
Blue waffle disease can not be transmitted to anyone. The disease is fictional. However, individuals should always be conscious of changes around or to their genitals to ensure they do not have a real STI.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more