How Long Can You Live After A Cystectomy?
WHAT IS CYSTECTOMY?
Cystectomy is a medical term for surgical removal of all or part of the urinary bladder. It may also be rarely used to refer to the removal of a cyst.
PURPOSE OF CYSTECTOMY
Cystectomy is the surgical procedure for:
- The removal of the urinary bladder.
- The removal of an abdominal cyst.
- The removal of cancerous organs close to the bladder.
TYPES OF CYSTECTOMY
The types of cystectomies include:
- Partial Cystectomy (also known as segmental Cystectomy).
This involves the removal of only a portion of the bladder.
This type involves the removal of the entire bladder together with surrounding lymph nodes and other nearby organs that contain cancer.
- Ovarian Cystectomy
This is the removal of the ovary along with the bladder as a result of ovarian cancer. In men, removing the entire bladder (Radical Cystectomy) always involve the removal of the bladder, the prostrate, and the seminal vesicles. In women, radical cystectomy also involves the removal of the uterus, ovaries, and part of the vagina.
The challenge of bladder removal is how the individual will manage their urine to a point of elimination. After bladder removal, your surgeon also has to create a urinary pathway – a new way to store and eliminate urine in your body. The surgeon also will decide which method is best for you.
The most common warranting removal of the urinary bladder is bladder cancer. Usually, Cystectomy is performed to treat invasive or recurrent noninvasive bladder cancer.
Cystectomy may also be used to treat other pelvic tumors (advanced colon, prostate, or endometrial cancer) and some noncancerous (benign) disorders (interstitial cystitis or congenital abnormalities).
Radical cystectomy is recommended for the treatment of bladder cancer that has invaded the muscle of the bladder (malignant). Also, individuals with a high risk of cancer progression or failure of cancer to respond to less invasive treatment (malignant) may benefit from cystectomy.
To choose the type of cystectomy to be performed, many factors are to be considered. Some of such factors may include:
- Type of cancer
- Baseline bladder function
- Location and size of the cancer
- Stage of the cancer
- Age of individual
- The overall health of an individual.
Partial Cystectomy
A partial cystectomy involves the removal of only one portion of the bladder and is performed for certain tumors (benign or malignant) localized to the bladder.
Candidature for partial cystectomy includes those with:
- Single tumors localized near the dome, or top of the bladder
- Tumors that do not invade the muscle of the bladder
- Tumors located within bladder diverticulum
- Cancer that is not carcinoma in situ(CIS).
- Tumors have originated and spread from neighboring organs such as the colon.
Radical Cystectomy
A radical cystectomy is mostly performed for cancer that has invaded the muscle of the bladder. Radical cystectomy involves the removal of the bladder along with the surrounding lymph nodes and other cancerous organs. In men, the bladder, prostate, and seminal vesicles are removed. In women, the bladder, uterus, fallopian tubes, ovaries, and a portion of the vagina are removed.
RISKS
Cystectomy is a complex surgery because it involves the manipulation of many internal organs in your abdomen. For this reason, Cystectomy involves certain challenging risks including:
- Bleeding
- Blood clots
- Infection
- Heart attack
- Pneumonia
- Dehydration
- Electro abnormalities
- Urinary tract infection (U.T.I)
- Bowel obstruction (food or liquid may be blocked from passing through your intestines.
- Ureter blockage (a blockage in one of the tubes that carry urine from the kidneys)
- Death can result after surgery – however, rare.
Some of these complications may be life-threatening and need necessary intervention. There may be a need for further surgery to correct some abnormalities, or you may need to be readmitted to the hospital.
Preparing For Cystectomy
Talk with your doctor about the medicines you take. Discuss with your doctor about your use of caffeine, alcohol, or other drugs (if any)
You may need to change your medications or drop certain practices or habits to help healing recovery after surgery and even before surgery. Quit drinking alcohol, quit smoking, they are at high risk of bladder cancer
You will receive specific instructions on how to prepare for the procedure. Study them for compliance. If you have questions about the instructions; follow up with your doctor. Plan to come to the hospital during cystectomy with somebody. Do not come with your valuables.
CYSTECTOMY PROCEDURE
Surgeons perform bladder removal surgery. They may choose one of the three different surgical approaches:
Open Cystectomy
- You will take general anesthesia that will make you asleep
- The surgeon will make one long incision in your abdomen to access your bladder and the tissues around it
- The surgeon ( and anesthetist)hands enter the body cavity to perform the operation
- The open portion is stitched back.
Minimally Invasive (Laparoscopic Cystectomy)
- You will take general anesthesia that will make you asleep
- The abdomen is first insufflated with carbon dioxide
- The surgeon makes several small incisions on your abdomen where surgical tools are inserted to access the abdominal cavity
- The surgeon’s assistants’ hands enter the body cavity to operate.
Minimally Invasive (Robotic Cystectomy)
- You will take general anesthesia that will make you asleep
- The surgeon makes several small incisions on your abdomen
- Surgical tools are inserted to access the abdominal cavity
- Your surgeon site at a console and remotely operates the surgical tools.
Reconstruction Of The Urinary Tract
In each of the three Cystectomy options, the surgeon will need to remove your bladder along with nearby lymph nodes. He may also need to remove other organs near the bladder, such as the urethra, prostate, and seminal vesicles (in men) and the urethra, uterus, and a portion of the vagina ( in women).
On removing your bladder, your surgeon works to reconstruct the urinary tract to create a pathway to allow urine to leave your body. Your surgeon may choose one of these several options;
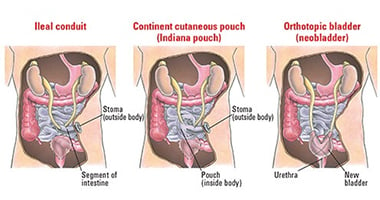
- Ileal Conduit
Your surgeon uses a piece of your small intestine to form a tube that attaches to your urethras connecting your kidneys to an opening in your abdominal wall (stoma), urine flows from the opening continuously and is collected in a bag you wear on your abdomen, which sticks to your skin until you drain it.
- Neobladder Reconstruction
Your surgeon uses a slightly larger piece of your small intestine than the used for the ileal conduit to form a sphere-shaped sac that becomes your new bladder. The neobladder is placed in the minimal bladder position inside your body and attached to the ureters, so that urine can drain out from your kidneys. The other end of the neobladder is attached to your urethra, allowing you to urinate in a relatively normal way. However, you might need to use a catheter to help better remove urine from the neobladder. Some people report an inability to continue urinating after surgery.
- Continent Urinary Reservoir
Your surgeon will use a piece of your intestine to form a small reservoir inside your abdominal wall. Your urine will subsequently drain into the reservoir. When the reservoir is filled, you use a catheter to drain the reservoir several times a day.
The advantage of the neobladder and urinary reservoir, over the ileal conduit, is that you avoid the need to wear a urinary collection bag on the outside of your body. But you’ll need a catheter to drain your urine several times a day. The pool of urinary diversion is to enable safe storage and timely elimination of urine after the bladder removal while preserving your quality of life.
After The Procedures,
You may need to stay in a hospital bed for up to 5 to 6 days. You may experience some side effects of the anesthesia, such as sore throat, sleepiness, shivering, dry mouth, nausea, and vomiting. These may go away after a few days.
In the mornings, your health care team may have you get up and walk to achieve a quick and full recovery. Pains from incisions may last for a few weeks but may heal off in course of time.
Before you leave the hospital, talk with your doctor about your medicine and other things you may need to improve your comfort.
RECOVERY
While back home, remember to keep follow-up appointments. Call on your doctor at any time you need to. Keep to all your drug prescriptions. Have regular walks to facilitate your healing. Take liquid foods, with much water until your doctor recommends otherwise.
Six to eight weeks after surgery, you may resume light activities such as bathing, driving, going back to work or school. Ask your doctor when to resume sexual activities. You may need adjustment in your style changes.
MORTALITY RATE
Radical cystectomy (RC) is a very complex urologic procedure. Despite the improvement in practice, technique, and process of care, it is still associated with significant complications including death, with reported postoperative mortality rates ranging from 0.8 percent to 8 percent.
FAQS
- How Long Can You Live After A Cystectomy?
Patients in group I achieve a progression-free 5years survival rate of 77% and an overall survival rate of 63% after 5 years. In group 2 patients achieved a progression-free survival rate of 51% after 5 years and an overall survival rate of 50%.
- Does bladder cancer spread fast?
High-grade bladder cancer is likely to grow and spread quickly and become life-threatening. High-grade cancers often need to be treated with chemotherapy, radiation, or surgery. Low-grade cancers appear non-aggressive and have a low chance of becoming high-grade. They are rarely life-threatening.
- Can you live a normal life without a bladder?
It can affect your body image, and you may worry about the impact on your relationships and sex life. With enough time, you should be able to do almost everything you did before. Even if you now use a urostomy bag (to collect your urine), you can go back to work, exercise, and swim.
- What can you not do after bladder surgery?
Avoid strenuous activities, such as bicycle riding, jogging, weight lifting, or aerobic exercises, for about 3 weeks, or until your doctor says it is okay. For about 3 weeks, avoid lifting anything that would make you strain.
- How long can you live after bladder removal?
The five-year survival rate after cystectomy is about 65 percent.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more