Flexible Sigmoidoscopy
Flexible Sigmoidoscopy is a diagnostic endoscopic procedure used for the examination of the lower part of the gastrointestinal tract, including the colon and rectum. It is one of the most accurate methods for examining the inner area of the anus, rectum, and colon (up to 60cm from the anal verge). It allows examination of the… Read More
Top Doctors For Flexible Sigmoidoscopy Treatments
Top Hospitals For Flexible Sigmoidoscopy Treatments
Flexible Sigmoidoscopy
Flexible Sigmoidoscopy is a diagnostic endoscopic procedure used for the examination of the lower part of the gastrointestinal tract, including the colon and rectum. It is one of the most accurate methods for examining the inner area of the anus, rectum, and colon (up to 60cm from the anal verge). It allows examination of the sigmoid colon, collection of biopsy samples, and detection of colon cancer at an early stage. The doctor uses a thin, flexible tube called the Sigmoidoscope for the procedure. The device is inserted through the anus into the rectum and then into the sigmoid colon. Such diagnostics are quite informative since it gives real-time visuals with the help of a camera attached to it and monitor. The doctor prescribes Sigmoidoscopy for symptoms such as abdominal pain, rectal bleeding, chronic diarrhea, and other intestinal problems. It does not allow to see all parts of the large intestine.
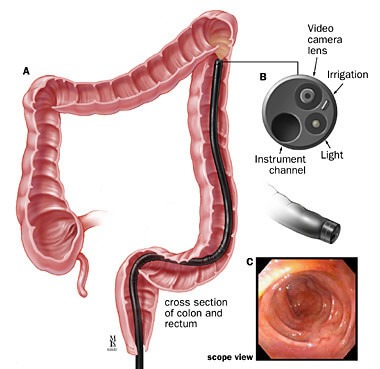
Why is Flexible Sigmoidoscopy performed?
The doctor recommends Flexible Sigmoidoscopy to examine intestinal signs and symptoms. Common reasons are:
- Determine the cause of rectal bleeding, diarrhea, constipation, lower abdominal pain, or inflammation
- To understand the cause of blood in stools, low blood count, and low iron level.
- As a screening test for polyps, ulcers or colon cancer
- To monitor your response to treatment if you have inflammatory bowel disease
- To detect colorectal cancer, strictures (narrowing of the colon), diverticula (small pouch on the colon wall)
- Sharp weight loss for unknown reasons
- To take a sample of tissue for examining it in detail (biopsy)
- In elderly patients, as a screening test for the prevention of bowel cancer
- As a screening test for colorectal cancer for men who are 50+
- As a primary procedure before colonoscopy
A clinical study in 2010 found that considering Sigmoidoscopy as a screening test after 50 years of age reduces the risk of colon cancer by 33%, and the mortality to 43%.
Flexible Sigmoidoscopy is not advised under the following conditions:
- Bowel perforation (hole in the lining of the intestine)
- Active peritonitis (inflammation of the peritoneum which covers the abdominal cavity)
- Cardio-pulmonary instability
- Inflammation of the colon
- Lack of good bowel preparation [1]
How to prepare for Flexible Sigmoidoscopy?
Usually, the doctor prefers to perform Flexible Sigmoidoscopy in the morning as the colon must be sufficiently empty for the doctor to see the intestinal wall. The doctor gives specific instructions on how to prepare for the test, which may include laxatives or enemas. On the day of the test, the diet should be mostly liquid, and not solid form.
The healthcare professional will provide specific instructions on how to prepare for the examination. Adhering to instructions gives maximum safety during and after the test, minimizes complications, and allows the endoscopist to examine the colon effortlessly.
Two factors to consider before the test:
- Colon cleansing: The patient must clean the lower part of the colon to allow the endoscopist to see the lining of the colon. Specific instructions will then be given for preparation often involving a liquid diet, taking a laxative, or using an enema shortly before the test.
- Medicines: Some medications, such as those containing a lot of iron, must be discontinued two weeks before the procedure. Iron covers the colon, making it difficult to see the lining. If the patient is taking these medications, they should ask their doctor if they need to stop taking them before the procedure. People who are taking blood-thinning medications such as warfarin (Coumadin) should talk to their doctor about the need to temporarily stop taking this medication. Most medicines for high blood pressure, heart disease, lung disease, thyroid medications, and seizures are safe during Sigmoidoscopy, and you can take it on the day of the exam. The patient may need to adjust diabetes medications before the test in consultation with their doctor.
It is necessary to read the following instructions in advance and follow them carefully. If the patient has questions, he/she should discuss them in advance with his/her doctor.
Preparation for the procedure includes the following action plan:
- For 72 hours before the test, bakery and confectionery products, milk, mushrooms, legumes, raw vegetables, fatty meats, fast food, alcoholic and carbonated drinks should not be consumed. Give preference to vegetable soups, porridge with water.
- Two to three days before the procedure, the patient needs to stop eating foods that have an intense red color like tomato juice, jam, berry jelly as they can mimic blood.
- In some cases, it is necessary to avoid some drugs, for example, blood thinners. But do it only after taking permission from a doctor.
- The day before the Sigmoidoscopy, dinner has to be avoided; only drinking water and liquid food are allowed.
- In the evening before and the next morning, 2-3 hours before the procedure, cleansing enemas are performed.
How Flexible Sigmoidoscopy Carried out?
Before the Sigmoidoscopy, the nurse will give instructions to make sure the patient understands the procedure. The doctor may do a body check-up to review the patient, including possible complications, and may ask the patient to sign a consent form after counseling the patient regarding the procedure thoroughly. The nurse may ask to wear a hospital gown. Unlike colonoscopy, Sigmoidoscopy is a less painful procedure, so the doctor often performs it without anesthesia.
Flexible Sigmoidoscopy usually takes 5 to 20 minutes. The patient lies on the left side (lateral position) and pulls the knees bent legs towards the chest. The doctor then inserts a lubricated tip of the sigmoidoscope into the anus. He slowly proceeds with the device, examining all parts of the intestine. At this time, the doctor asks us to lie still, not moving. There may be discomfort since the tube also inflates your colon with some air to facilitate examination. Patient may experience cramps, muscle cramps, or lower abdominal pain. You may feel to have a bowel movement. Inform the doctor if you experience severe pain.
During the process, you may ask to adjust the positions & take deep breaths to make it easy. After removing the sigmoidoscope, you need to lie down for several minutes and then get up slowly, without sudden movements.
A doctor may take a small piece of tissue (biopsy) for further examination. Taking a biopsy does not cause pain or discomfort to the patient. The entire procedure is usually easy to carry over.
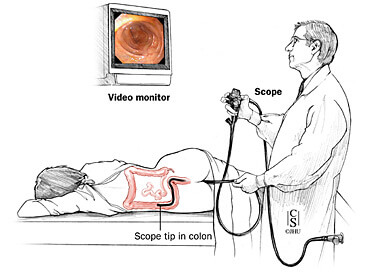
What happens post-Flexible Sigmoidoscopy?
Post Sigmoidoscopy, you can return to normal activities, including eating. In many cases, the patient can go to work and drive the same day, provided that there are no complications. A sedative pill (if given) will make you feel sleepy, so it’s better to consult your doctor before resuming daily activities. You can continue other medications and diet as directed by your doctor.
The sample of tissue, if removed, will be sent to the laboratory for examination. The result may take 1-2 weeks. You may also need to carry out other tests depending on the results obtained. The doctor will call you to discuss the results of biopsies if taken. You need to repeat the procedure if your doctor was unable to get a good picture of your colon and rectum. Talk to your doctor about any questions or concerns regarding your colorectal health or results.
rs for Flexible Sigmoidoscopy?
Flexible Sigmoidoscopy is a safe procedure compared with colonoscopy, and complications are infrequent. Firstly, the device is not inserted fully inside the large intestine, and the doctor can better control its movements. Secondly, you remain conscious and can feel discomfort.
Sometimes minimal bleeding occurs with biopsy or removal of polyps. The device can cause a tear or hole in the tissue during an examination.
Sigmoidoscopy is limited to screening the lower part of the intestine. A complete screening for colorectal cancer requires a colonoscopy. If you are experiencing the following symptoms, consult a doctor as soon as possible:
- Bleeding per rectum after the procedure, which lasts more than a day(more than a teaspoon of blood)
- Black, tarry stools
- Severe abdominal pain
- Heavy bowel movements, constipation
- Signs of infection, including fever or chills
- Nausea and vomiting
- Inability to pass gas or stool
- Chest pain or shortness of breath
References: