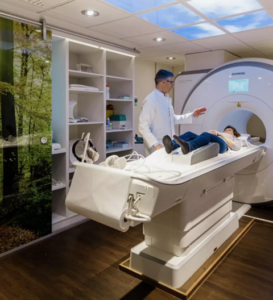
Magnetic Resonance Cholangiopancreatography (MRCP)
[lwptoc] Overview Magnetic resonance cholangiopancreatography (MRCP) is a non-invasive medical imaging technique that utilises very powerful magnetic resonance imaging, alongside radio waves, and a computer to visualize and assess the biliary, pancreas, bile ducts, gallbladder and pancreatic ducts for diseases. The MRCP procedure is also used to determine if gallstones are lodged in any of… Read More
Top Doctors For Magnetic Resonance Cholangiopancreatography (MRCP) Treatments
Top Hospitals For Magnetic Resonance Cholangiopancreatography (MRCP) Treatments
Magnetic Resonance Cholangiopancreatography (MRCP)
[lwptoc]
Overview
Magnetic resonance cholangiopancreatography (MRCP) is a non-invasive medical imaging technique that utilises very powerful magnetic resonance imaging, alongside radio waves, and a computer to visualize and assess the biliary, pancreas, bile ducts, gallbladder and pancreatic ducts for diseases. The MRCP procedure is also used to determine if gallstones are lodged in any of the ducts surrounding the gallbladder. It does all these without the use of ionizing radiation. MRCP offers radiologists the ability to analyse source images, and 2 and 3-dimensional projections.
The MRCP procedure, however, has a couple of limitations, such as low sensitivity of the ultrasound for detecting common duct calculi. This means that the diagnosis of several common conditions such as calculi, tumours (benign and malignant), sclerosing cholangitis and chronic pancreatitis may still require invasive procedures like endoscopic retrograde cholangiopancreatography, ERCP, or percutaneous trans-hepatic cholangiography, PTC.
Why an MRCP diagnosis may be required?
An MRCP procedure may be requested to help diagnose pancreatic cancer and/or cancer of the bile duct. It is also frequently used in the diagnosis of called primary sclerosing cholangitis. A condition commonly associated with inflammatory bowel disease and causes the narrowing of the bile ducts.
An MRCP diagnosis is also recommended to help define the severity of certain conditions or to find out whether there are complications.
Magnetic resonance cholangiopancreatography has also proven to be a safer alternative to the more invasive test called endoscopic retrograde cholangiopancreatography, ERCP, Which makes use of endoscopy, contrast medium and X-rays. The invasive nature of ERCP makes it risky. Some of the associated risks with ERCP include inflammation of the pancreas, infection, bleeding and perforation of the bowel or bile duct.
Preparation for an MRCP Diagnosis Procedure
It is usually recommended that those patients undergoing an MRCP diagnosis fast for at least 4 hours prior to the MRCP procedure. This is to help with the reduction of gastro duodenal secretions, reduce bowel peristalsis and related motion artefact, and to promote distension of the gallbladder that may occur during the MRCP procedure.
Patients are also not allowed to wear any jewellery or metal hair accessories during an MRCP scan, and their clothing will be replaced by a hospital gown.
Those who experience fear for confined spaces or anxiety, or are worried about how they will feel being in an enclosed space during the test may be given a mild sedative before the test. However, some MRI scan machines are open on the sides and maybe more tolerable for those with anxiety.
An MRCP scan machine is quite noisy, so reduce headphones or earplugs is usually provided to protect the ears from noise. MRCP scan is usually not recommended during pregnancy, especially during the first 12 weeks. So if you are pregnant, tell the doctor or the radiographer (the medical imaging specialist) so that extra precautions can be taken.
Procedures involved in a magnetic resonance cholangiopancreatography
The patient is made to lie very still in an MRI scanner for several minutes at a time. Although the machine is quite noisy, you, however, won’t feel anything during the scan procedure, and the entire procedure should be done within less than 20 minutes.
For an MRCP test, a contrast medium (that is, the special dye that highlights certain areas on scans) is not usually needed. However, when it is given, it is given intravenously, through a drip into a vein.
After all prerequisites have been done, the MRCP procedure then gets started.
Magnetic resonance imaging, MRI that is, uses radiofrequency waves concentrated at the body to excite hydrogen atoms in the molecules of water in the body. This is carried out in a very strong magnetic field, which causes the protons in the nuclei of the hydrogen atoms to line up, instead of being randomly positioned. Upon return to their natural alignment, these protons then emit radio signals. The signals are what is used to build a computerised image that shows differences in body tissues based on the amount of water in them. This allows extremely clear and detailed images to be obtained.
The aftermath of the procedure
After a magnetic resonance cholangiopancreatography, you will be made to wait while the images are checked and to know if more images may be needed.
If a sedative was given before the MRCP procedure it is advisable that you don’t drive, operate machinery, or make important decisions until the sedative wears off completely.
The associated risk with magnetic resonance cholangiopancreatography
Magnetic resonance cholangiopancreatography, MRCP, is generally very safe. It uses a magnetic field, and so there is no exposure to radiation.
There is, however, a small risk of an allergic reaction to the contrast medium that is sometimes used. Those with severe kidney disease are not able to have contrast medium as it causes, though rarely, organ damage in these people.
Limitations of magnetic resonance cholangiopancreatography.
The ability of an MRCP scan to generate high-quality images depends on your ability to remain perfectly still and follow the breath-holding instructions while the images are being recorded. Therefore, the inability to lie still during the imaging may lead to low-quality images.
MRCP scan machines often come with weight limits. Therefore, a person who is very large may not fit into certain types of MRI machines that are used.
Implants and other metallic objects make it challenging to get clear images.
Irregular heartbeats may also affect the quality of images generated as some of the techniques time the imaging based on the electrical activity of the heart.
Even though there is no evidence to prove that an MRCP scan harms the foetus. It is advisable that pregnant women should not have an MRCP diagnosis during their first trimester unless medically essential.
FAQs
Is MRCP with or without contrast?
For a magnetic resonance cholangiopancreatography, a contrast medium may or may not be required. However, when it is required, it is given intravenously through a drip.
Is fasting required for an MRCP?
Yes. Patients undergoing an MRCP test fast for 4 hours prior to the MRCP procedure to reduce gastro duodenal secretions, reduce bowel peristalsis and related motion artefact, and to promote distension of the gallbladder.
Why may I be requested to carry out an MRCP test?
The MRCP test may be requested of you can be for evaluation of several pancreatic biliary ductal system conditions. Some of which include:
- To identify congenital anomalies of the cystic and hepatic ducts.
- To evaluate post-surgical biliary anatomy and complications
- To diagnose pancreas divisum
- Anomalous pancreatic biliary junction
- To evaluate for choledocholithiasis
- Biliary strictures
- To evaluate trauma to the biliary system
- To detect the cause of narrowing or blockages in the bile duct or the pancreatic duct.
- To detect tumours in the bile or pancreatic duct.
The MRCP test may also be used to determine the cause of:
- Chronic pancreatitis (that is, inflammation of the pancreas) and pancreatic cystic lesions.
- Jaundice.
- Upper abdominal pain.
- Liver disease.
How will I get my MRCP results?
After the MRCP procedure, a radiologist (a medical specialist in imaging) reviews, analyses and interprets your results. After which it will be sent to your doctor. Your doctor will be the one to explain the outcome of the findings and give you the results.
What is the difference MRCP vs. ERCP
MRCP is a non-invasive medical imaging technique and uses a powerful magnetic field, radio waves and a computer to visualize and evaluate the biliary, pancreas, bile ducts, gallbladder and pancreatic ducts for diseases.
While ERCP uses a combination of fluoroscopic imaging and luminal endoscopy in its procedures for diagnosis and treatment.
Does an MRCP scan uses radiation?
A magnetic resonance cholangiopancreatography uses a very strong magnetic field, and not ionising radiation. This also means that people with some types of metal objects in their body system cannot take this test.
So if you have any of the following in your body, such as an artificial heart valve, cardiac pacemaker or defibrillator; metal clips used to close off an aneurysm (an expanded blood vessel); a joint replacement; a cochlear (inner ear) implant; metal coils in blood vessels; or any other metal objects, it is advisable you mention it to the doctor.