Prostate Cancer
Prostate Cancer has some alarming statistics associated with it being crowned the most common in males, second only to skin cancer in the United States. For reasons unknown, black and Hispanic men run a higher risk of being diagnosed of prostate cancer compared to their white counterparts. Although being the third largest reason for cancer deaths in the US, it has a relatively high 5 year survival rate (percentage chance of the patient living for more than 5 years after diagnosis) of nearly a 100 per cent with the rate dropping to 96 per cent in the 15 year mark.
It is to be noted that this is not the case when the cancer in question has spread from the prostate gland to the rest of the body, in which case the rate drops to 29 per cent. Numbers aside, prostate cancer is a serious issue and a threat to men everywhere.Situated below the bladder and in front of the rectum, the prostate gland is a part of the male reproductive body that secretes seminal fluids in charge of providing nutrition to the sperms produced by the testis. Besides this, the prostate gland is involved in urine control given that it uses its muscle fibres to control the flow of urine passing through the urethra, which passes through the centre of the gland. A cancer in this region means that the gland cells present in it are now abnormal with it diving and expanding in an uncontrolled manner, a type of prostate cancer called adenocarcinomas.This is the most common type of prostate cancer with other types like Sarcomas, Neuroendocrine tumors etc. existent but extremely rare. If you have prostate cancer, it is most definitely adenocarcinomas, and throughout this article we will be referring to this type of prostate cancer.
Symptoms
Prostate cancer is a slow progressive disease, with the symptoms extremely unclear. The cancerous alterations formed in the gland cells, called Prostatic intraepithelial neoplasia (PIN) are believed to be an ideal factor for assessing the nature of the cancer in the gland. It is believed that nearly 50 per cent of males aged 50 are said to have it. In extreme cases, older men (and sometimes young men) who have died due to other causes were revealed to have prostate cancer in their autopsy report. Prostate cancer is a silent disease, with no symptoms shown in its early stages or none at all, with diagnosis usually made during routine medical check-ups. Symptoms do exist, they may include the following: – Patient would urinate more often, with him getting up in the middle of the night to urinate. – Find it hard to start urinating and continue urinating. – Urination may be painful and there may be blood in the urine.
Given that no symptoms show up in the early stages, the first sign that the patient may have prostate cancer is on the basis of how high his/her PSA levels are in their blood. Prostate specific Antigen or PSA for short is a protein produced in the gland that helps keep the semen in liquid form. A common misconception is that a high PSA level maybe harmful to you. This is not the case, as a high PSA level only means that something is wrong with the gland. It also doesn’t mean that one has cancer as there are various other reasons why he/she may have such high levels. For instance, male hormone altering medication is prone to affect the levels of PSA as there is a positive correlation between male hormones and the size of the prostate gland. With a bigger the prostate gland, the levels of PSA are bound to rise. The bigger prostate gland, on the other hand, may block the urethra passing through it, thereby causing problems while passing urine. This condition, called Benign Prostatic Hyperplasia (BPH) although shares symptoms with prostate cancer, is not cancerous in nature. It is still a serious issue and must be treated immediately.
Staging:
With the PSA levels’ indicating an issue with the prostate gland, the next step is to see if prostate cancer is the issue in question. In light of this, two categories of systems are available to not only confirm the presence of prostate cancer but also determine the affected regions. TNM (Tumor/Nodes/Metastasis) is a system used to identify the stage of cancer in the prostate gland and the area affected by it. It denotes the stages of the cancer with respect to the tumor (T), the Lymph nodes (L) and distant organs/tissues of the body (M). Each category is numbered from 1 to 4 where each successive number represents the size and/or spread of the cancer in the prostate gland and nearby regions. Same number scheme is followed in the Lymph Nodes and the distant organs. The Gleason Score is similar to TNM, a pathologist will determine the existence and the extent of a cancer via your biopsy samples. Then they will grade it on a scale of 2 to 10 with 2 being the least and 10 being the highest.
Risk Factors
Though no one knows the exact causes that lead to prostate cancer, certain factors may play a role. Age: older the individual, the more likely he is to get prostate cancer. The risk is lower with men less than the age of 45 but higher and more common after the age of 50.
Genetics: Studies indicate that the risk of getting prostate cancer is higher if a close family member was also diagnosed with it.
Diet: An unhealthy lifestyle and diet could also increase the chances of prostate cancer
Sexually transmitted diseases (STD): Patients who had a history of Gonorrhoea are more prone to be diagnosed with prostate cancer.
Treatment
Treatment for prostate cancer varies between each case on the basis of the stage and level of the cancer in question. However the treatments that are available for prostate cancer come with a catch. To say that men undergoing the treatments will be able to live normal lives is an understatement as they come with various complications like erectile dysfunction and inconsistency in urine flow. In light of this doctors may try to approximate the number of years the patient is likely to live for. If it is over 10 years, active surveillance is preferred which involves the doctor monitoring the cancer in fixed intervals with the help of various diagnostic tests like blood tests aimed at determining the amount of PSA in the blood and DRE (Digital Rectal Examination) which involves inserting a gloved and lubricated finger into the rectum to look for irregularities and the presence of a tumour and in certain cases, a prostate biopsy.
If the patient develops any of the symptoms or his cancer has reached a dangerous state, then local treatments will be recommended. On the other end of the spectrum, with individuals suffering from other conditions along with prostate cancer along with a life expectancy lower than 10 years, doctors try to avoid the tests mentioned in the case of an active observation method and take a watchful waiting approach. What this involves is not performing any of the tests or treatments until the symptoms start to reveal itself. Especially in the case of older men (over the age of 60), performing tests and treatments with that sort of outlook has been shown as ineffective than doing nothing. Also, the treatments sort, when the symptoms show up, are not localized but systemic in nature as chances are the cancer has spread throughout the body and requires treatment that is not specific or local to a specific area. These two kinds of treatment are discussed below.
Localized Treatment:In cases where the cancer is restricted to just the prostate gland and has not spread to any other area of the body, localized treatments are chosen.
They include:
Surgical Options: The goal of a surgical procedure with respect to prostate cancer, is to safely remove the affected region (in this case the prostate gland) and some of its neighbouring healthy tissue so as to disallow the cancer from metastasizing any further. Based on how invasive the surgery is and the procedure used, there are two types of surgeries that may be on the table:
Radical (open) prostatectomy: Involves the use of relatively larger incisions: retropubic/suprapubic (lower abdomen) incision or perineum incision (through the skin between the scrotum and the rectum). The former is used in cases where the neighbouring lymph nodes and/or nerves have been affected and require removal along with the entire prostate gland and seminal vesicles. The latter, although not used as commonly as the former, may be preferred if the cancer has left the nerves and lymph nodes unscathed and is also a more faster procedure.
Robotic or Laparoscopic prostatectomy: Unlike its open counterpart, a laparoscopic prostatectomy involves smaller incisions, less bleeding and faster recovery time. The procedure involves the surgeon making small keyhole incisions and inserting various cameras and robotic instruments designed in the form of tubes, to remove the prostate gland and its surrounding healthy tissue. Success/Survival Rate- The choice between these two depend on a case by case basis and a lot of factors come into play. Although a laparoscopic procedure is less invasive and has better recovery times than its open counterpart, both of them have the same side effects which include urinary inconsistency and erectile dysfunction, which may be rectified via medication or further medical intervention. Also, studies have shown that both procedures have statistically, the same success rates and post-surgery medical intervention rates, meaning that the choice of surgery would depend upon the patient’s condition and the skill of the surgeon or the equipment available in the chosen hospital (laparoscopy requires robotic instruments, which a few may not have). Still, the best way to choose is to ask and discuss with your doctor about what is best suited for you.
Radiation Therapy: Simply put, these procedures involve making use of high intensity rays to kill the cancer cells present in your prostate and its surrounding area. How your radiation oncologist may go about it, depends on your case and the facilities available to you. Common radiation practises include:
External beam radiation therapy: The most commonly used radiation procedure, this involves making use of high intensity x-rays directed at the specific region with the help of a machine outside the body. To increase accuracy, some hospitals may have Conformal Radiation Therapy (CRT) machines and procedures available, which with the help of computers, maps the exact area of the cancer and directs the rays there, thereby not affecting and compromising the healthy tissue surrounding it.
Intensity modulated radiation therapy (IMRT): Similar to the previous case, differentiates itself from an external beam radiation therapy by making use of CT scans to map the location and characteristics of the cancer and developing a 3D image. From this, the radiation oncologist uses variable beams of radiation to treat that specific area depending on the amount of cancer and healthy tissue in that region. Also poses a significant lower risk of damaging any of the neighbouring healthy tissue.
Proton Therapy: Unlike external beam radiation therapy, this procedure makes use of high intensity protons instead of x-rays. However it is to be noted that proton therapy has no significant advantage over conventional x-ray beam therapy and is also more expensive.
Brachytherapy: With the help of a catheter, high intensity radioactive sources are called seeds are inserted into the area surrounding the cancer so as to kill the cells. Relatively more advanced than other procedures, it is used alongside other procedures like external beam therapy or androgen deprivation therapy (ADT). These seeds may be in low or high doses depending on your individual case: for low doses, the seed is usually kept in the body for along time and can work for about a year whereas high intensity seeds may be placed in the body for about thirty minutes.Focal Therapy: Though not established as a standard procedure, focal therapies are those that use heat/cold to kill cancer cells in the region. Cryotherapy is one such procedure, which involves probing the affected region with a metal stick and freezing it. However, the side effects of this treatment haven’t been completely explored and defined.
Systemic Treatments:Mainly used in cases where the cancer has spread beyond the prostate gland and/or the patient is older than sixty years. The procedures include:
Androgen Deprivation Therapy (ADT): Prostate cancer, especially in its early stages, depends on various androgen like testosterone to grow. Androgens are hormones that help the prostate gland to grow and the body to develop. With ADT, the goal is to cut the supply of androgens to the tumour thereby restricting the growth of the cancer. This is done by either removing the gland that produces testosterone- the testicles or via medication. The side effects of this type of therapy may only last for the tenure of the therapy. However in cases of surgically removing the testicles (also called surgical castration), the side effects may remain longer. These include: erectile dysfunction, loss of body mass, loss of sexual desire,depression, weight gain etc. However, such treatment is only possible until the cancer becomes castration- resistant or when the effects of ADT are nil on the cancer.
Chemotherapy: Involves the use of certain kind of drugs aimed at killing the cancer cells. With respect to prostate cancer, these drugs are introduced to the body by intravenous(IV) means. Chemotherapy has various side effects which include and are not limited to: bleeding, vomiting, hair loss, diarrhea etc. However, the side effects depend from person to person and no two individuals will have the same side effects. It is thus necessary for the patient to let the doctor to know about the side effects when they occur so that he/she can provide the necessary medication to counter or at the very least, soothe the symptoms. It is also crucial to take rest while on chemotherapy, as the drugs tend to be powerful and works best under low stress, both mentally and physically.
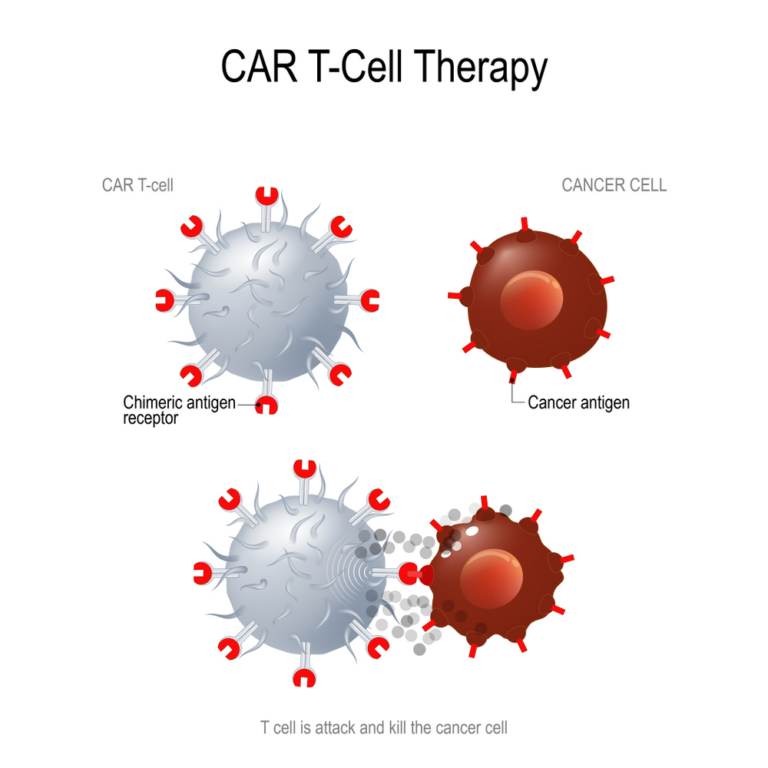
Immunotherapy: This treatment procedure is usually used alongside other treatments and involves using drugs to facilitate the immune system to fight against the cancer cells. The white blood cells or specifically the T cells are in charge of attacking any alien cells in the body. Cancer cells usually get away scott free because they’re based on the normal cells which are now mutated. This allows them to avoid the wrath of the T cells and grow freely. However, with immunotherapy, the T- cells are given the ability to detect the cancer cells and fight them. Side effects may be mild and include headache, nausea and body pain.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more