Autoimmune Pancreatitis (AIP)
Autoimmune pancreatitis is an uncommon disorder that causes the immune system to attack healthy cells of the pancreas. It occurs when the immune system triggers swelling and inflammation of the pancreas. Read More
Top Doctors For Autoimmune Pancreatitis (AIP) Treatments
Top Hospitals For Autoimmune Pancreatitis (AIP) Treatments
Autoimmune Pancreatitis (AIP)
Table of contents
- What is autoimmune pancreatitis?
- What are the types of autoimmune pancreatitis?
- Causes
- What are the risk factors associated with autoimmune pancreatitis?
- Symptoms
- How is autoimmune pancreatitis diagnosed and treated?
- What are the complications of autoimmune pancreatitis?
- What is the life expectancy of autoimmune pancreatitis?
- FAQ
What is autoimmune pancreatitis?
Autoimmune pancreatitis (AIP) is an uncommon disorder that causes the immune system to attack healthy cells of the pancreas. It occurs when the immune system triggers swelling and inflammation of the pancreas.
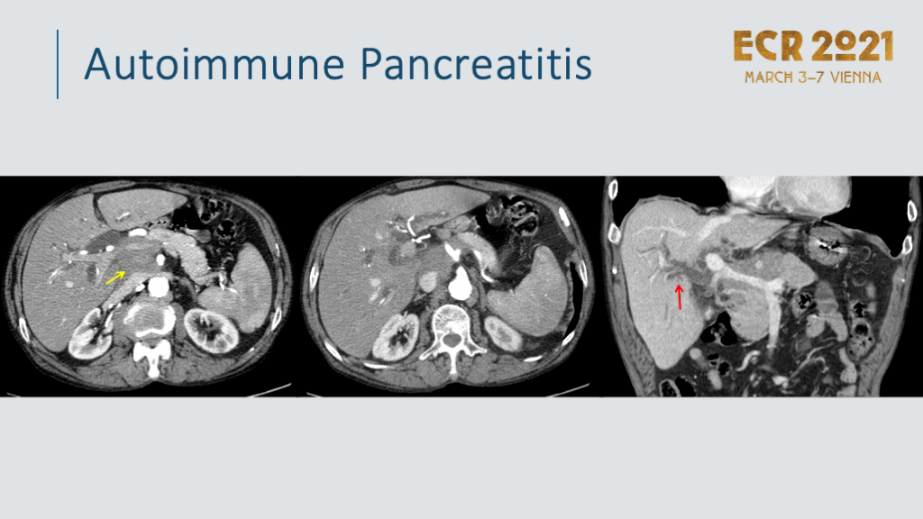
What are the types of autoimmune pancreatitis?
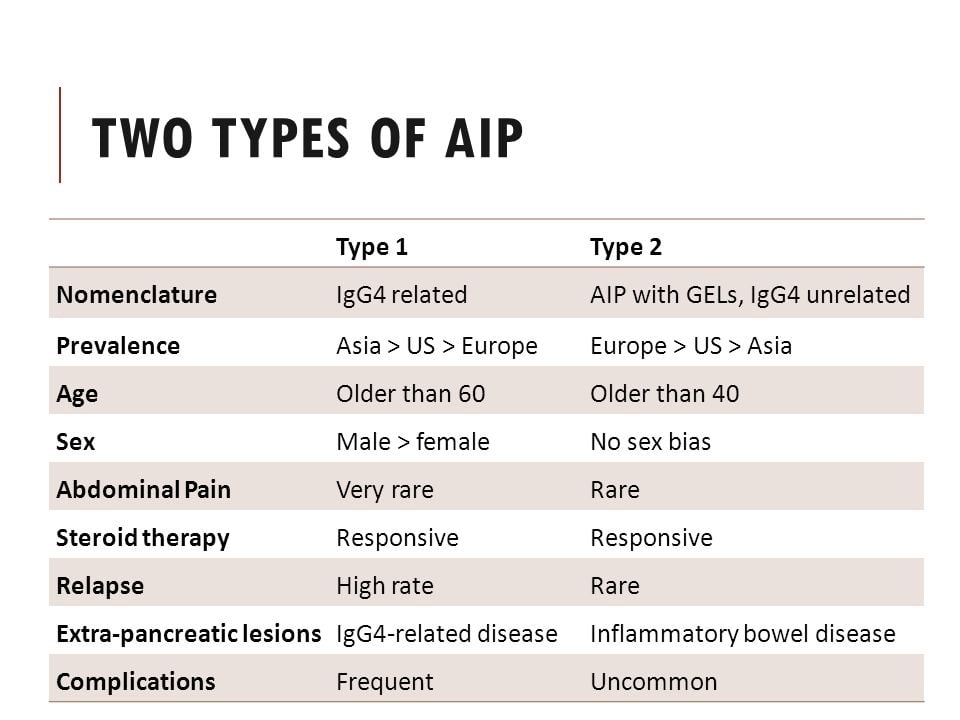
There are two types of autoimmune pancreatitis, and they are as follows:
- Autoimmune Pancreatitis Type 1: It is a very common type of AIP. It affects the pancreas as well as other organs in the body, which include the liver as well as the gallbladder. This type of AIP responds well to steroid treatment. Type 1 AIP also has the probability of relapse if the treatment is discontinued.
- Autoimmune Pancreatitis Type 2: Type 2 AIP is associated with inflammatory bowel issues or disease
Causes
Doctors actually don’t know what exactly causes autoimmune pancreatitis. However, in certain other autoimmune cases (diseases), the body’s immune system actually affects the healthy body tissue.
What are the risk factors associated with autoimmune pancreatitis?
The risk factors of Autoimmune Pancreatitis based on types are as follows:
- Type 1: People over 60 years and especially men, are at high risk of getting the disease
- Type 2: People over 40 years, men and female, have a high risk of having inflammatory bowel diseases like ulcerative colitis
Symptoms
The symptoms of autoimmune pancreatitis are as follows:
- Jaundice
- Growth or mass in the pancreas
- Stomach ache
- Loss of weight
- Backache
- Extreme tiredness or fatigue
- Dark urine
- Pale stools
- Vomiting and nausea
- Appetite loss
How is autoimmune pancreatitis diagnosed and treated?
Autoimmune pancreatitis disease usually involves the following diagnostic procedures,
Prior to the Treatment:
- The diagnosis of autoimmune pancreatitis is challenging to analyze since most of the signs and symptoms are similar to pancreatic cancer. To determine the diagnosis for the type of AIP a person has, the doctor will advise the patient to take a blood test and imaging tests before the treatment.
- There is no single diagnostic test to confirm autoimmune pancreatitis. A combination of blood tests, imaging tests, and biopsy are done to confirm the condition.
- Blood test- They include a complete blood count, liver function test, and immunoglobulin test in which elevated levels of IgG4 are seen. People with type 1 AIP have increased levels of IgG4, whereas those with type 2 AIP do not.
- Imaging tests- They include CT scan, MRI scan, endoscopic ultrasonography, and ERCP (endoscopic retrograde cholangiopancreatography). These scans help in identifying abnormalities in the pancreas.
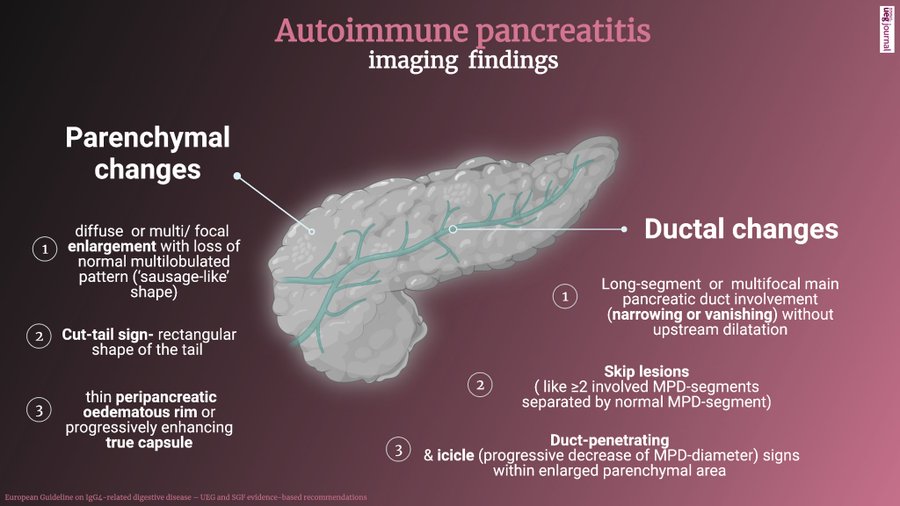
- Endoscopic core biopsy– During this procedure, a thin, flexible tube is inserted through the mouth, into the stomach, and pancreas under the guidance of ultrasound. The doctor takes a small sample of tissue and sends it for pathological studies. AIP has a very distinctive appearance which can be detected easily under the microscope.
- Steroid trial- Most patients diagnosed with AIP respond well to steroids.
During the Treatment:
- Biliary stent- To drain the biliary ducts, also called biliary stenting, the doctor will insert a small tube in people who have the symptoms of jaundice.
- During cases where steroid treatment is not effective, drainage will be recommended.
- Steroids- patients diagnosed with AIP often feel symptomatically better after a short course of steroid (prednisolone or prednisone) treatment.
- Steroid-sparing drugs- Additional treatment to help minimize the side effects that are associated with prolonged steroid use, doctors will often add drugs that can suppress or modify the immune system. It is at times called asteroid-sparing medications.
- Immunosuppressants or immunomodulators include azathioprine, mycophenolate, mercaptopurine, and rituximab. They are generally used to minimize the side effects associated with extended steroid use.
- Supplementary enzymes will also be prescribed by the doctors, such as Creon, Pancreaze and Pertzye.
Prognosis, Post-Treatment, and Recovery:
- The patient will be advised to carry on with steroid therapy for many years in order to stop the signs and symptoms from appearing.
- The doctor will monitor the patient continuously, although the signs and symptoms go away entirely with the help of steroid therapy.
What are the complications of autoimmune pancreatitis?
A few of the complications of autoimmune pancreatitis are as follows:
- Pancreatic Insufficiency: Autoimmune pancreatitis usually might affect the pancreatic ability in order to make more enzymes. Few signs such as diarrhea, weight loss, and metabolic bone disease will be the complications.
- Diabetes: Since the pancreas produces insulin, AIP may cause diabetes. It might need treatment either with oral-based medication or through insulin.
- Pancreatic calcifications or stones.
- Osteoporosis
- Fluid retention
What is the life expectancy of autoimmune pancreatitis?
Autoimmune pancreatitis usually does not affect life expectancy. In most cases, certain people will be advised to continue steroid therapy for many years to keep symptoms from returning. Apart from that, with successful management, individuals with the disease can live active as well as healthy lives.
FAQ
High protein and nutrient-rich diets, such as fruits, vegetables, whole grains, and other lean protein sources, are the diet for autoimmune pancreatitis.
IgG4-positive plasma cells are usually considered to be the marker for AIP. It is usually detected in the pancreas as well as in a variety of many tissues. Besides that, serum IgG4 levels are usually elevated to two times more than the upper limit, which is normal in most patients.
Carbonic Anhydrase as well as Lactoferrin. Apart from that, Anti-CA-IIAb and anti-LF antibodies are the very most detected antibodies in AIP.
No, individuals treated for AIP or autoimmune pancreatitis have a very normal life expectancy.
Findings that suggest autoimmune diseases other than pancreatic cancer include fluctuating obstructive jaundice and high or elevated serum IgG4 levels. However, both are not the same, though they mimic each other.
Autoimmune pancreatitis is a rare condition, occurring in less than 1 in 1,00,000 population. It accounts for only 2% of all chronic (long-lasting) pancreatitis [1].
No, since the exact cause of autoimmune pancreatitis is not known, hence it cannot be prevented.
References



























































































