Diverticulitis
WHAT IS DIVERTICULITIS? Diverticulitis is an inflammation or infection in one or more small pouches in the digestive tract. Diverticulitis is the most serious type of diverticular disease that has caused uncomfortable symptoms to people and, in some cases, serious complications. Before the 20th century, the diverticular disease was a rare occurrence, but now diverticulitis […] Read More
Top Doctors For Diverticulitis Treatments
Top Hospitals For Diverticulitis Treatments
Diverticulitis
Table of contents
What is Diverticulitis?
Diverticulitis is an inflammation or infection in one or more small pouches in the digestive tract. It is the most serious type of diverticular disease that has caused uncomfortable symptoms and, in some cases, causes serious complications. Before the 20th century, the diverticular disease was a rare occurrence, but now diverticulitis has become a serious health problem, a group of conditions affecting the digestive tract. If left untreated, the complication arising from this disorder can cause long-term health problems.
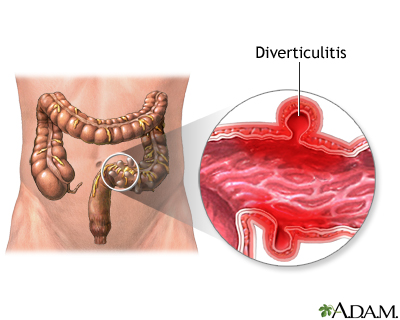
Causes
The diverticular disease develops when pouches (sac-like swellings) form along the digestive tract (particularly the large intestine). These pouches (known as diverticula) form when a weak spot in the intestine wall bulges outwards.
Diverticulitis is a condition where diverticula become inflamed and perhaps infected. This is likely when feces or partially digested food blocks the opening of the diverticula.
The health condition in which diverticula flare up along the lining of our digestive tract is known as diverticulosis. Still, it is called diverticulitis when the diverticula are inflamed or infected. In other words, it is only associated with inflamed or infected diverticula.
What are the risk factors of Diverticulitis?
- Genetics.
Diverticulitis may be hereditary.
- Age.
The risk of developing diverticulitis increases with age.
- Dehydration.
Not drinking enough water makes digestion difficult, and waste may not pass through the colon so easily.
- Smoking.
Nicotine and other chemicals in tobacco products can weaken the colon lining, resulting in diverticulitis development.
- Medication.
Certain drugs such as nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, and steroids may weaken or irritate the large intestinal walls. Ibuprofen (ADVIL, Motrin IB, others) and naproxen sodium (Aleve) must be avoided.
- Obesity.
People with extra weight can put more pressure on their colon.
- Straining when pooing.
This could put pressure on the walls of the colon.
- Lack of exercise.
Regular exercises tend to decrease the odds of developing diverticulitis.
- Nutrition.
Diet high in animal fat and low in fiber seems to increase the risk.
Symptoms
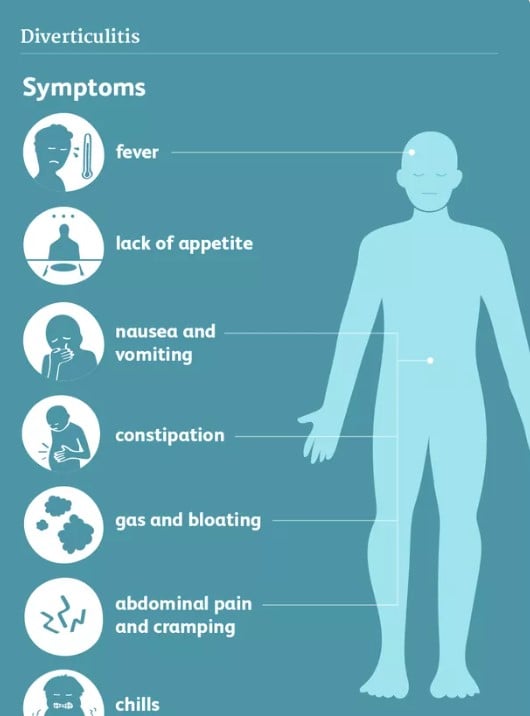
Diverticulitis can trigger symptoms that range from mild to very severe. The symptom may appear abruptly; however, in most cases, the symptoms develop slowly over time.
Potential symptoms of diverticular disease include:
- Bloating
- Constipation
- Diarrhea
- Fever and chills
- Nausea and vomiting
- Constant or severe abdominal pain
- Rectal bleeding
- Blood in the stool
- Crumpling on the left side of the abdomen may go after passing gas or having a bowel movement
- Attacks of infection
- Inflammation
- Bowel obstruction

How is Diverticulitis Diagnosed?
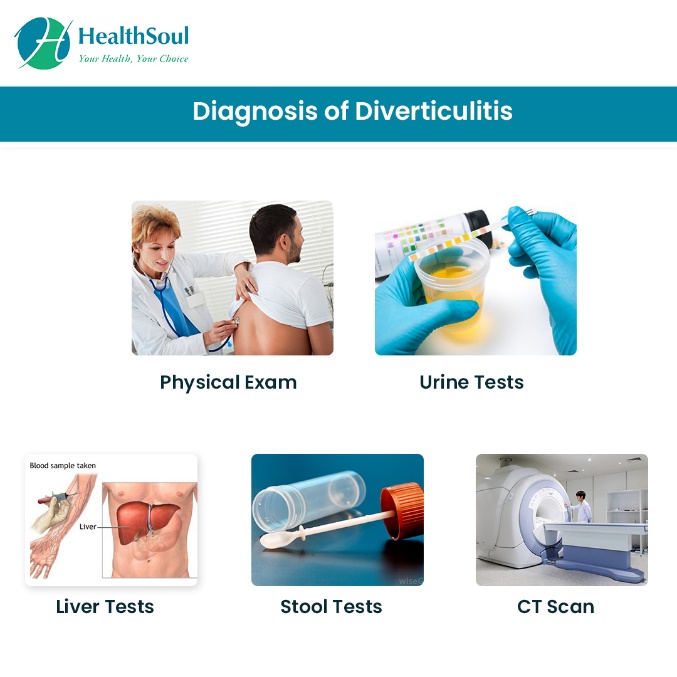
The diagnosis of diverticulitis is made during an acute attack. The doctor will perform a couple of tests to confirm the disease.
- Physical examination – During a physical examination, the doctor will examine the patient thoroughly to look for any abnormalities.
- Medical history – The doctor will record the medical history of the patient. History of any surgery or medication history.
- Family history
- Investigational scans- They include a CT scan of the abdomen. CT scans can help detect the pouches that are infected or inflamed and help confirm the diagnosis.
- Laboratory tests- complete blood count, liver function tests, urine tests.
- Pregnancy test – To rule out pregnancy as the cause of abdominal pain.
- Stool test to rule out infections in those with diarrhea.
How is Diverticulitis treated?
Mild diverticulitis can be treated with rest, changes in the diet, and antibiotics. Chronic or severe cases could require surgery. In complicated cases, the patient may likely be hospitalized. Treatment can involve:
- Antibiotics for diverticulitis include mesalazine [Asacol], rifaximin [Xifaxan], etc.
- Intravenous antibiotics
- Insertion of a tube to drain an abdominal abscess if any has formed
The doctor may recommend surgery if the patient is suffering from :
- Serious complications include a puncture (perforation) in the bowel wall, a bowel abscess, a fistula, or obstruction in the bowel wall.
- A weakened immune system
- Had multiple occurrences of uncomplicated diverticulitis.
Surgery
There are two main surgery options:
Primary Bowel Resection
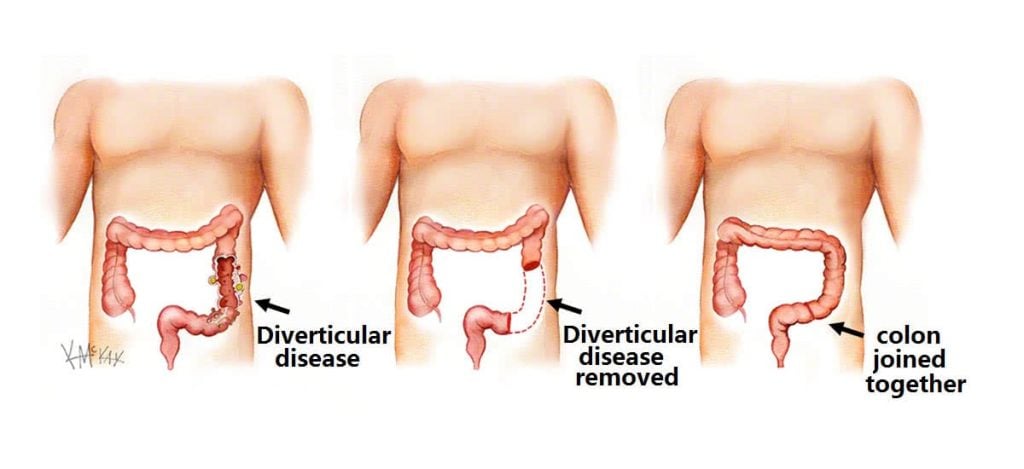
During this procedure, the affected parts of the intestine are removed, and the healthy ones are connected (anastomosis). This allows patients to experience regular bowel movements.
Bowel resection with colostomy
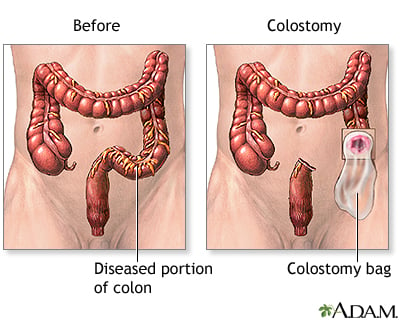
Whenever a patient has severe inflammation that seems impossible to rejoin the colon and rectum, the surgeon will perform a colostomy.
How?
A hole inside the abdominal wall connects to the healthy part of the colon by which waste is able to pass through the opening and into bags. When there is no irritation, the colostomy could be removed, and the bowel could be reconnected.
How to treat Diverticulitis at home?
When diverticulitis is mild, one can easily handle it at home, but when severe, it is advisable to be handled by professionals. Home remedies for diverticulitis include:
- High-fiber food helps to control symptoms or problems in people with diverticulitis.
- Drink lots of fluid, especially water.
- Eat fruits.
- Exercise often.
- Make sure to stay away from alcohol and smoking.
Complications associated with Diverticulitis
About 25% of patients with acute diverticulitis develop complications which may include:
- An abscess occurs when pus collects in the pouch
- A blockage in the bowel caused by scarring
- A fistula (an abnormal passageway) between sections of the bowel or bowel and other organs
- Peritonitis occurs if an inflamed or infected pouch rupture spills intestinal contents into the abdominal cavity.
- Strictures
Can Diverticulitis be prevented?

One may prevent it through the following:
- Eating more fiber. Food such as fresh fruits, vegetables, whole grains, seeds, and nuts.
- Drinking plenty of fluids.
- Exercise regularly. Make sure you exercise a minimum of 30 minutes per day.
- Avoid alcohol and alcoholic beverages, or at least reduce them.
- Avoid smoking. It can have harmful effects on the digestive system
- Maintain a healthy weight.
- Use a stool softener to reduce the pressure on the colon.
FAQ
The most common symptom is a sharp cramp-like pain, usually on the left side of the lower abdomen. Other symptoms include chills, fever, nausea, vomiting, and constipation or diarrhea.
In some cases, diverticulitis can be genetic, found in transferrable genes. That means that it can be hereditary.
Diverticulitis usually develops when naturally weak places in the colon give way under pressure. The result is that the pouches are marble-sized and extend through the colon’s wall. Diverticulitis can occur when the diverticula tear, which can cause inflammation and, in certain cases, even infection.
Avoid the following foods to divert from diverticulitis:
1) Certain fruits, such as apples, pears, and plums
2) Dairy-based foods, like yogurt, ice cream, and milk
3) Fermented foods, such as sauerkraut or kimchi
4) Beans
5) Cabbage
6) Brussels sprouts
7) Onions and garlic
The doctor may recommend the following treatment:
1) High fiber diet. While a diet high in fiber may not prevent the development of diverticulitis, it can help prevent the symptoms or cause of concern for those who already suffer from diverticulosis.
2) Fiber supplements, like methylcellulose (Citrucel) or Psyllium (Mechanical)
3) Medicines, such as mesalazine [Asacol], rifaximin [Xifaxan], etc.
4) Probiotics, such as yogurt.
5) Colon resection.
6) Abscess.
7) Perforation.
8) Peritonitis.
As the person gets older, the colon wall can become weaker. This can cause small pockets or pouches to form in weakened areas of the colon. If the pouches become infected, it could trigger an outbreak of diverticulitis or even flare-ups.
Diverticulosis – It means the presence of tiny bulges or pockets (also known as diverticula) in the intestines (colon). They are usually asymptomatic (no symptoms) and need no treatment. However, diverticulosis can lead to diverticulitis.
Diverticulitis means inflammation (swelling) and infection of one or more diverticula. The patient may experience abdominal pain, nausea, fever, and other symptoms. 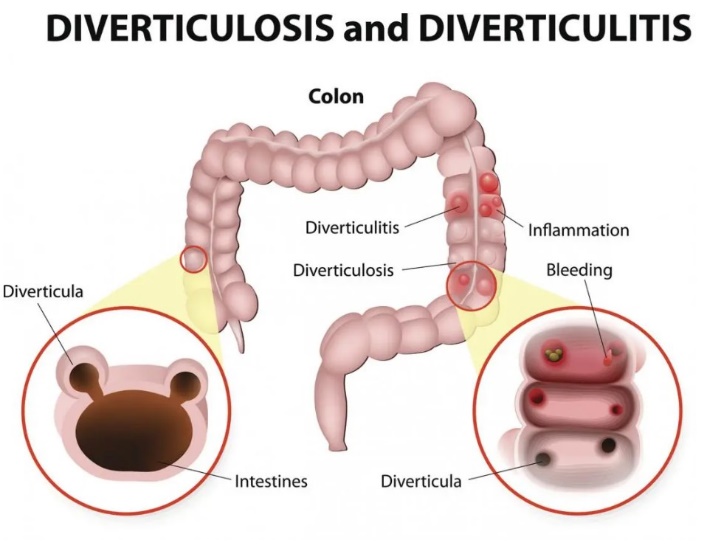
Picture Courtesy: medicalnews
Diverticulitis associated with life-threatening conditions are:
a) Rectal bleeding
b) Obstruction and strictures in the intestine
c) Abscesses and fistulas
d) Perforation leading to peritonitis.
Diverticulitis can be treated and healed with antibiotics at an early stage. The patient might require surgery in complicated cases. However, diverticulitis is generally considered to be a lifelong situation [1].
The surgical indications for diverticulitis are:
a) Tear (perforation) in the colon.
b) Uncontrolled sepsis
c) Abdominal or pelvic abscess
d) Intestinal obstruction
e) Failure of medical therapy
f) Fistula formation [2]
The outcome or prognosis of diverticulitis depends on the severity of the illness, the presence of any complications, and any underlying medical conditions. However, early diagnosis and early treatment will result in a good prognosis.
References
- https://my.clevelandclinic.org/health/diseases/10352-diverticular-disease
- https://www.medscape.com/answers/173388-20357/what-are-the-surgical-indications-for-diverticulitis



























































































