Hypereosinophilic Syndrome
Hypereosinophilic is an uncommon blood-related condition, when the count of eosinophils (WBC) unnaturally overproduces (above 1.5 * 10000 L) in more than 6 months, and destroys organs of the body. WBC or white blood cells function to protect the body’s immune system against infection and eosinophils comes in the category of WBC. Hypereosinophilic syndrome predominantly […] Read More
Top Doctors For Hypereosinophilic Syndrome Treatments
Top Hospitals For Hypereosinophilic Syndrome Treatments
Hypereosinophilic Syndrome
Table of contents
What is hypereosinophilic syndrome?
Hypereosinophilic syndrome is an uncommon/rare blood-related condition when the count of eosinophils (WBC) unnaturally overproduces (above 1.5 * 10000 L) in more than 6 months and destroys organs of the body.
WBC or white blood cells protect the body’s immune system against infection, and eosinophils come in the category of WBC. Hypereosinophilic syndrome predominantly affects the skin, heart, bone marrow, nervous system, and lungs. Peripheral eosinophils typically elevate; hence the disorder is idiopathic.
This syndrome largely affects men between the ages of 20-60. In a healthy person, the count of eosinophils is around 500-600 per microlitre. Broad names of this syndrome are lymphocytic and myeloproliferative. Children and women have negligible (very less) chances of this disorder. Chronic hypereosinophilic syndrome can result in myocardial fibrosis, heart failure, and death. Ethnicity isn’t involved in this disease.
What are the complications of hypereosinophilic syndrome?
- Parasitic infection
- Thrombus formation
- Chromosomal Abnormalities
- Heart valve thickens
- Endomyocardial fibrosis
- Alkaline phosphatase level increases
What are the risk factors associated with hypereosinophilic syndrome?
- A person whose body doesn’t fight against infection
- Incidence is higher in males.
- Affects the age between 20-60 years.
- History of blood cancer
- History of rheumatic diseases
- Repetitive skin diseases
- Family history of having hypereosinophilic syndrome.
How is hypereosinophilic syndrome treated?
The treatment aims to normalize the eosinophil count, reduce skin diseases, and arrange chromosomes in order. The treatment type relies on the patient’s symptoms, their cause, the organ/organs damage level, and on conducted tests.
If no serious symptoms exist, monitoring and medicines are considered excellent options. Medicines like:
- Gleevec (imatinib)
- Vincristine
- Hydroxyurea – Droxia, Siklos, Hydrea
A complete examination is done to minimize the chances of organ damage.
If the heart or nervous system isn’t functioning in the way it should, then Prednisone will be prescribed by a doctor. Usually, this syndrome thickens the blood, so to neutralize it, warfarin or heparin is given most of the time.
Other medications include :
- Etoposide
- Arevincristine
Surgery For Hypereosinophilic Syndrome
Surgery becomes essential when nothing works, and the damaged organs begin to damage other body organs. The doctor selects multiple surgery options according to the patient’s health and the damaged organ.
- Valve Replacement Surgery
This surgery increases the life expectancy of a patient by 90-95%. When single or all the four valves stops responding due to this syndrome. The huge incision (cut) will be made from the neck to the umbilicus (belly button). A cut can be shorter depending on the severity, and then another cut will be made in the aorta to remove the damaged valve and replace a new one. The surgery has minimal chances of death, about 1-2%, and also this surgery regulates accurate blood circulation.
- Thrombectomy
When the syndrome is diagnosed in a patient’s body, it starts interrupting blood consistency by making it thicker, and eventually, blood clotting starts. During this procedure, the surgeon puts an intravenous cannula on the patient’s hand, and warfarin or heparin will be injected. The incision will be made around blood vessels, remove the clotted blood, then the area will be closed with sutures, and normal blood flow starts.
- Bone Marrow Transplant
Damaged bone marrow will be replaced with a new one by adding new and working stem cells. This surgery is the most chosen one.
- Splenectomy – When the spleen is causing blood-related disorders in a patient, the doctor either treats the particular area or removes a portion or entire spleen.
How is hypereosinophilic syndrome diagnosed?
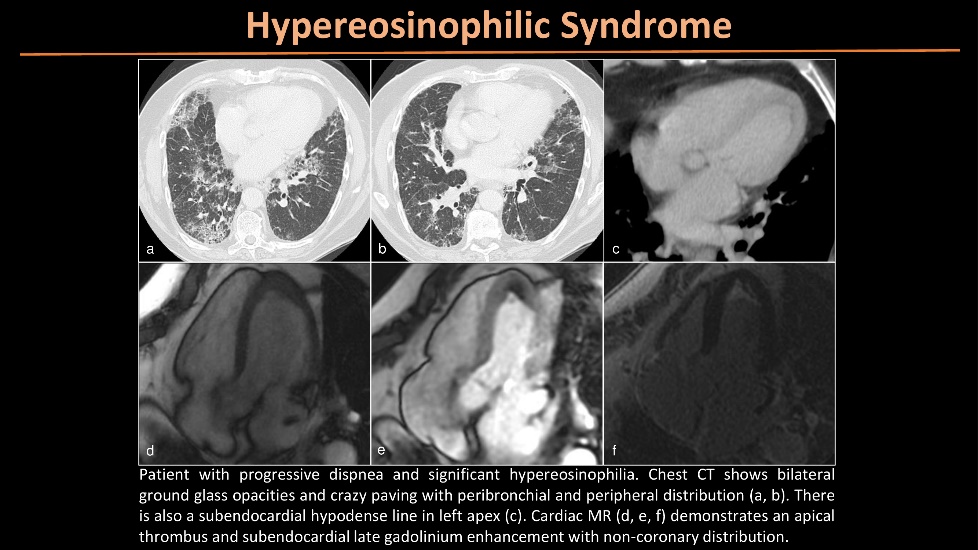
Patients should clear their medical history to pursue the diagnosis.
Tests that are performed during analyzing of this disorder are:
- Electrocardiogram
- Spirometry – to check the health of lung
- Computed Tomography – It thoroughly monitors the spleen, bone marrow, and chest
- Blood tests – To know about infections
- Chest X-ray
- Cytogenetic Test
- CT scan
- To detect the gene mutation – genetic tests are available
- Pulmonary function test
- MRI Scan
Symptoms
The symptoms associated with hypereosinophilic syndrome are listed below:
- Skin itching and redness
- Abdominal pain
- Joint and muscle pain
- Fever
- Chest pain
- Fatigue
- Rhinitis
- Shortness of breath
- Cough
- Blurry vision
- Dizziness
- Night sweats
- Irregular bowel movements
- Nausea
Symptoms depend upon the age and which part of the body is connected with this syndrome.
Causes
The actual cause is still not known, while a few of the causes are listed below:
- Drug/medicine allergy
- The mutation of genes, generally called a familial hypereosinophilic syndrome, results from some family history.
- Clonal Myeloid malignancy, myeloproliferative disorder.
- High levels of interleukin-5
- Elevation of protein
- Addison’s disease
- Skin diseases like dermatitis
- Helminthic disease
- Sarcoidosis
- Leukemia
- Bone Marrow disorders
However, it is not sure that all these things are causing this syndrome, but still, research is saying that this can worsen the eosinophilic numbers.
FAQ
No, hypereosinophilic syndrome cannot be prevented.
The prognosis of this syndrome depends upon variable factors. In severe or chronic cases, it can be fatal if left untreated. However, initial studies have shown that hypereosinophilic syndrome carries a poor prognosis of survival rate of 3 years in 12% of the cases. Early diagnosis and treatment will improve the patient’s quality of life.
Hypereosinophilic syndrome is considered a chronic and progressive disorder that is potentially fatal. However, early diagnosis and treatment can improve the patient’s quality of life.










































