Inflammatory Bowel Disease
Inflammatory Bowel Diseases can be very chronic with several complications. The causes remain unknown but there are a couple of risk factors. Treating IBD may include medications and surgeries. It is important to know all about it as anyone is at risk of developing the disease.
Inflammatory Bowel Disease (IBD) is a term that encompasses the disorders that cause severe inflammation of the digestive tract, which includes the esophagus and the small and large intestine.
Read MoreTop Doctors For Inflammatory Bowel Disease Treatments
Top Hospitals For Inflammatory Bowel Disease Treatments
Inflammatory Bowel Disease
Table of contents
- What is inflammatory bowel disease?
- What are the types of inflammatory bowel disease?
- Causes
- What are the risk factors for inflammatory bowel disease?
- Symptoms
- How is inflammatory bowel disease diagnosed?
- How is inflammatory bowel disease treated?
- Possible Complications of IBD
- Can inflammatory bowel disease be prevented?
- FAQ
What is inflammatory bowel disease?
Inflammatory bowel disease, also called IBD, is chronic and prolonged inflammation (pain and swelling) of the digestive tract.
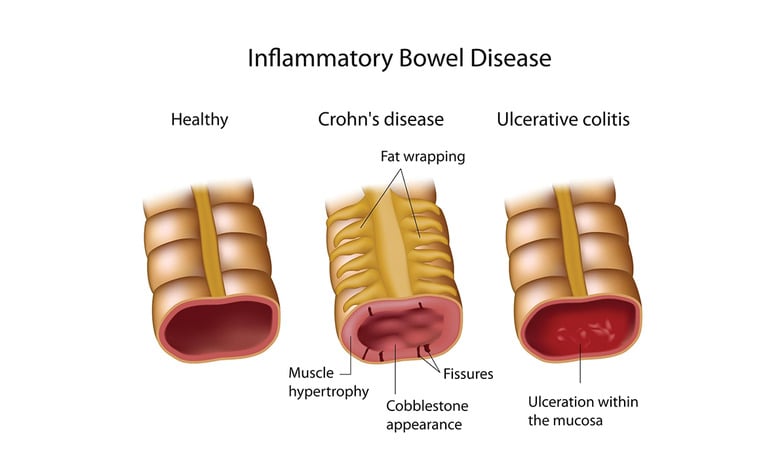
What are the types of inflammatory bowel disease?
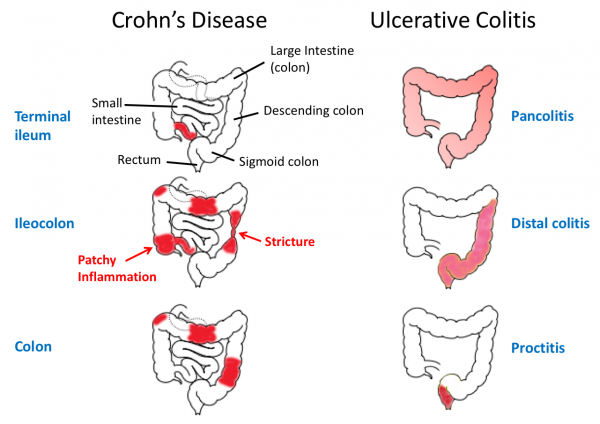
Inflammatory bowel disease is of two main types:
- Ulcerative Colitis (UC)
This inflammation spreads continuously, usually beginning from the rectum and more adversely in the large intestine (colon). The inflammation often brings out ulcers in the inner linings of the colon, hence the name ‘ulcerative colitis.’
There are different types of ulcerative colitis, which are based on their location and the state of severity. Some include; ulcerative proctitis, pancolitis, proctosigmoiditis, distal colitis, and acute ulcerative colitis.
- Crohn’s Disease (CD)
This inflammation occurs in any part of the digestive tract, from mouth to anus. It affects the small intestine first before spreading to the large intestine (colon).
Unlike ulcerative colitis, it is not a continuous spread but affects the digestive tract in patches. That is, inflamed tissues mix themselves with healthy tissues.
Causes
The triggering cause of IBD is unknown. There is no exact explanation of what triggers the digestive tract’s inflammation. However, research has stated that a couple of factors play a role in kicking off IBD.
Bacteria, viruses, antigens, or even our body’s tissues cause an autoimmune response to produce inflammatory reactions. There could also be environmental or genetic factors.
But whichever it is, IBD is mostly based on factors that could start reactions rather than causes.
What are the risk factors for inflammatory bowel disease?
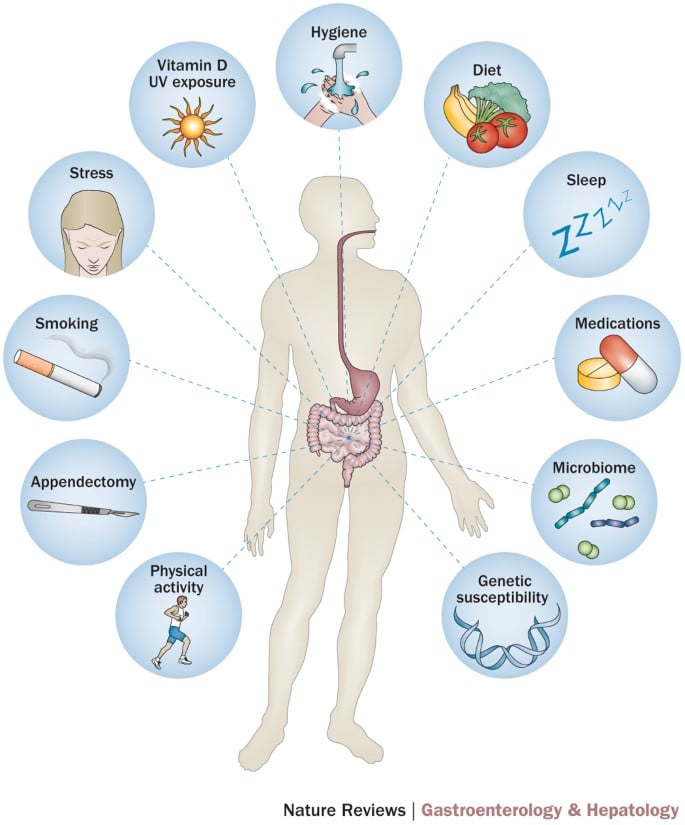
The risk factors of inflammatory bowel disease are listed below:
a) The Immune System
There are several ways the immune system can contribute to digestive tract inflammation.
- Fight Against Infectious Attacks.
The body is created in such a way that on the attack of a bacterial or viral infection, in which the immune system, as a controlling factor, produces pathogens that fight these infections. When this infection is in the digestive tract, the fight against it is engaged, and the tract can be inflamed due to the reactions. But when the infection dies off, the inflamed tract heals up.
- Autoimmune Response
This is a defect that occurs whenever our body’s immune system begins to attack our own body cells. As a result, our immune system begins to attack the digestive tract tissues, causing inflammation.
- Weak Immunity
If a person has an immunodeficiency, then the body’s immune system is too weak to fight against the infectious attack in the digestive tract. The bacteria, viruses, and antigens attack the tract with no resolution, and this causes inflammation.
b) Environmental Factors
Geography and places of habitat can contribute to IBD.
- Urban Areas
Suppose a person lives in urban and industrialized areas. In that case, they will be exposed to chemicals, materials, and diseases that can affect the digestive tract, making the person at higher risk of having IBD.
- Cold Climates
In areas of cold climates, there’s a high risk of having inflamed digestive tracts.
c) Lifestyle
Certain lifestyle choices affect our digestive tract causing IBD.
- Diet
Foods that contain a high level of fat and calories heighten the risk of IBD. High cholesterol causes inflammation in the digestive tract. Caffeine also affects the tract.
- Smoking
Smoke is not healthy for the digestive tract; it inflames the pathways. Added with high nicotine, the risk of having IBD is way higher.
d) Medications
Drugs such as nonsteroidal anti-inflammatory drugs (NSAIDs), antibiotics, birth controls, abortion pills, hard drugs, etc., have substances that cause inflamed tracts and, in turn, cause IBD.
e) Physiology
Physiological attributes can contribute to IBD.
- Age
Although Inflammatory Bowel Disease can happen to anyone of any age, it is mostly triggered from age 20 and adversely affects people over 60 years.
- Gender
IBD affects all genders. However, ulcerative colitis happens more in the male gender, while Crohn’s disease occurs mostly in females.
f) Family Traits
The traits transferred through generations can be a contributory factor in IBD.
- Genetics
No particular genetic strand can be linked to IBD, but research has discovered that people with a parent, sibling, or relation with the disease are most likely to have the disease themselves.
- Ethnicity
IBD has been attributed to certain decennaries or ethnic groups. For example, Jewish descents with particular emphasis on the Ashkenazi and the Caucasian tribes.
Symptoms
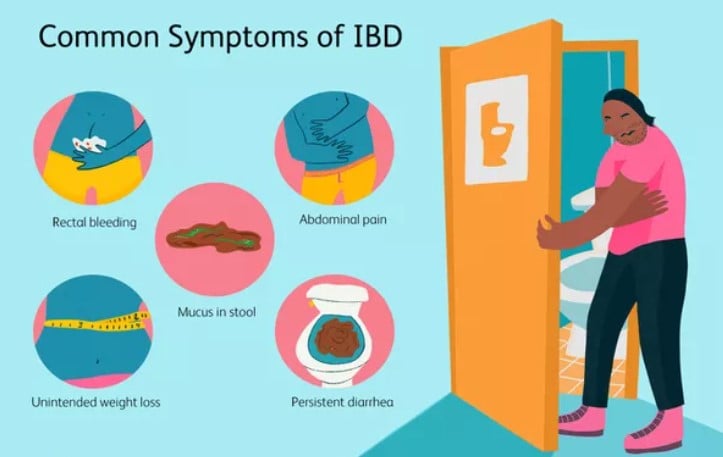
IBD symptoms play out differently based on the location and severity of the inflammation. Some include:
- Fever
- Fatigue
- Severe abdominal cramps and pains
- Bowel obstruction or blockage.
- Hematochezia, bloody stools.
- Diarrhea
- Anemia
- Loss of appetite
- Weight loss
- Sores in mouth, genital area, and/or anus.
- Painful menstruation in females
- Joint pains
- Skin disorders
- Arthritis, etc.
How is inflammatory bowel disease diagnosed?
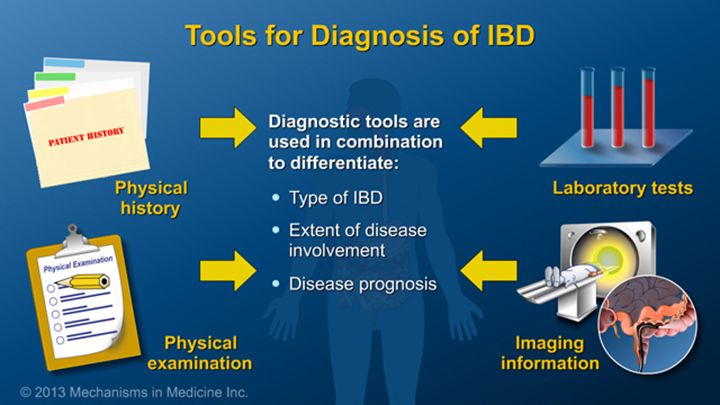
Whenever the person has started noticing some of the signs associated with IBD, then the person must consult a doctor immediately. Sometimes the signs may be from another disease, and the doctor is there to make certain what is causing those symptoms.
On visiting a doctor, the doctor will go through the patient’s medical and family profile and history. The doctor will advise the patient to undergo a couple of tests to confirm the disease.
Some of these tests include:
- Stool sample
- Blood tests
- CTs and MRIs to run a full detailed image of the tract.
- X-rays, such as barium enema, check the damage’s extent.
- Biopsy; where a small part of the intestinal wall will be taken and examined.
- Endoscopic procedures use inserted cameras to get a view of the digestive tracts. Some include:
- Upper Endoscope; a flexible tube along with a camera is inserted to examine the esophagus, abdomen, and the first part of the small intestine.
- Colonoscopy; inserted to examine the entire large intestine.
- Flexible Sigmoidoscopy; inserted to examine the last sections of the large intestine.
- Capsule Endoscopy; swallowed to enable the doctor to examine the small intestine, which is the toughest part to examine.
How is inflammatory bowel disease treated?
Several ways exist to suppress the symptoms, achieve remission, and prevent complications. These ways include:
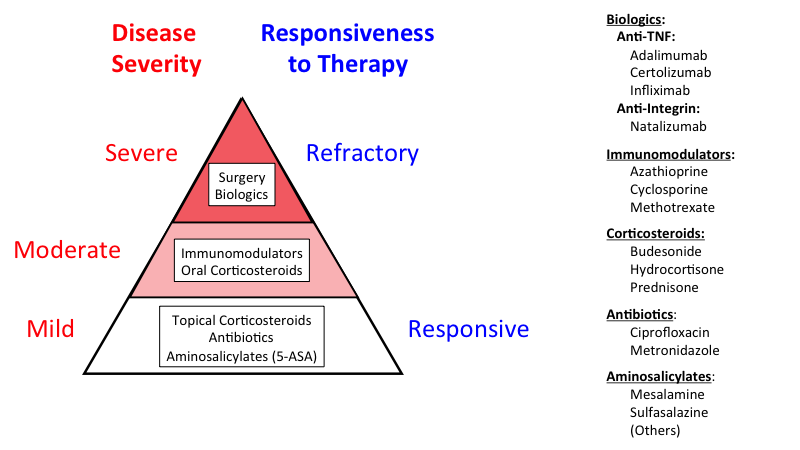
1. Medications
The doctor prescribes drugs according to the severity of the IBD. They include:
- Anti-inflammatory Drugs
They reduce flare-ups and help maintain remission, but long-term use can worsen the symptoms. Therefore, if milder NSAIDs are ineffective, fast-acting ones should be used to enable short-term use. Mesalamine, sulfasalazine, corticosteroids, etc., are types of anti-inflammatory drugs.
- Immune Suppressants or Modulators
These drugs stop the body’s immune system from attacking the bowel’s tissue and cells, which in turn causes inflammation. They should be taken for the short-term, advisably 3 months, to avoid side effects such as a risk of infection.
- Biological Therapies
These drugs are antibodies that fight against certain substances that cause flare-ups in the digestive tract.
- Antibiotics
Antibiotics kill bacteria or viruses that may trigger or make aggressive digestive tract inflammations.
- Anti-diarrheal drugs and laxatives
These drugs reduce the effects and symptoms of inflammation.
2. Lifestyle
Factors or habits in our life can make the IBD symptoms worse. Changes in these areas can help manage the symptoms and put the disease in remission.
a) Diet
Our diet matters a lot in trying to curb IBDs.
- Reduce the intake of fatty foods, spicy foods, high fiber foods, and dairy products.
- Eating small bits, rather than having a large quantity at a go.
- Avoid caffeine and alcoholic drinks.
- Drink a lot of water and stay hydrated.
- Take vitamin and mineral supplements to avoid or control nutritional deficiencies.
b) Stress
The patient tends to experience more severe symptoms whenever they are stressed. To manage the stress level, engage in:
- Therapeutic exercises such as yoga.
- Meditation to ease the inner mind.
- Breathing exercises
- Recreational activities
- Hobbies.
c) Smoking
Smoking is a severe risk factor for digestive tract inflammation. First, the smoke is harmful, and then the nicotine, tobacco, and other substances contained in the cigarettes are high triggers to flare-ups. Therefore, to control IBD, the patient has to quit smoking if it is a habit.
3. Surgery
In severe cases of IBD, surgeries may be needed. Some surgeries include:
- Closure of fistulas or perforated intestine.
- Widening of narrowed bowels through strictureplasty
- If the patient is diagnosed with Crohn’s disease, then the affected parts of the intestines can be removed.
- For ulcerative colitis, the entire large intestine and rectum can be removed.
Possible Complications of IBD
There are several complications associated with IBD. These cases arise when the effects of IBD have been going on for a while and could be life-threatening. They include:
- Severe diarrhea
- Toxic megacolon; widening and swelling of the large intestine.
- Bowel obstruction, as inflamed parts of the bowel swells and thickens, blocking the rectum.
- Ulcers in the digestive tracts, including the mouth, anus, and genitals.
- Fistulas in the gut and anus.
- Intestinal perforations or ruptures.
- Rectal bleeding was found on stools.
- Anemia due to rectal bleeding.
- Colon cancer
- Osteoporosis; bone fractures due to bone density reduction.
- Anal fissures; tears in the tissue lining of the anus.
Can inflammatory bowel disease be prevented?
Since the main causes of IBD are unknown, the risk factors may not be insurmountable but can be controlled.
The ways to reduce the risk of developing inflammatory bowel disease are as follows :
- Controlling the diet and eating healthily
- Stop smoking
- Exercise regularly to relieve stress
Inflammatory bowel diseases are very discomforting and come with severe pains. The complications can be destructive to vital body parts, so one should control and plan what to do not to develop them or carefully manage them when it arises.
FAQ
Often, a person who has Crohn’s disease is rather constipated than having diarrhea since the affected area is the small intestine. The area becomes inflamed, and swelling builds up, causing the intestine to be constricted and narrow. This leads to bowel obstruction.
Inflammation in the digestive intestine can -not be cured but can go into remission. And it can take days to months for this remission to happen, depending on how early the treatment starts. It is therefore important to consult early with the doctor for the best treatment.
In remission, symptoms will go away, and the person will feel better, but that doesn’t mean the inflammation is completely gone. The person needs to keep up with healthy practices to prevent the symptoms from appearing again. The suppressed inflammation can still show with the use of endoscopic scans and tests.
Alcohol contains substances that irritate the digestive tracts, which will worsen the state of the disease. So, as an IBD patient, it is advisable that one should reduce their consumption of alcohol and, if possible, stop it.
Having IBD does not mean the patient cannot work. As a way to keep managing and controlling the symptoms from getting severe till they go into remission, the patient can keep working. But still, the patient has to do it at a minimal level because stress can increase the rate of inflammation.
Complications associated with ulcerative colitis are:
a) Toxic megacolon
b) Perforated colon (hole in the colon)
c) Excessive diarrhea resulting in chronic dehydration.
Complications associated with Crohn’s disease are:
a) Bowel obstruction
b) Malnutrition
c) Anal fissures (tear in the tissue that lines the anus or the skin around the anus)
d) Fistulas (abnormal connections between different parts of the body)
Yes, there is a possibility that a person can suffer from both at the same time.



























































































