Nasal Polyps
Nasal polyps are noncancerous growths of the lining of the tissues in the nose or mucosa. These noncancerous growths result in corpulent swellings in the lining of the mucosa and nasal sinuses consisting of the air-filled space directly connected to the nasal cavity. These nasal polyps are painless and soft, and they cling to the lining like a drop of tears. Read More
Top Doctors For Nasal Polyps Treatments
Top Hospitals For Nasal Polyps Treatments
Nasal Polyps
Table of contents
What are nasal polyps?
Nasal polyps are noncancerous growths of the lining of the tissues in the nose or mucosa. These noncancerous growths result in corpulent swellings in the lining of the mucosa and nasal sinuses consisting of the air-filled space directly connected to the nasal cavity. They are painless and soft, and they cling to the lining like a drop of tears. They are a result of an inflammation said to be chronic, and they are linked to infections, asthma, drug sensitivity, allergies, or even specific immune disorder.
Cases of nasal polyps can be severe or mild, the symptoms are insignificant when it is mild, but when it is severe, they can lead to blockage of the air-filled space resulting in infection, shortage of breath, and even the inefficiency of the sense of smell. Nasal polyps can be yellowish-brown or pink, and as they swell, they migrate from teardrops size to that of a grape on a stem. They can develop in either one or both sides of the nose, clustering separately or accumulatively. Anyone is susceptible to nasal polyps, though; it occurs more commonly in middle-aged or adults, mostly in men than women. Certain medications can be taken to exterminate the condition when it is mild, and in severe conditions, surgery might be required since the swelling tends to be recurring even after successful treatment.

Causes
The main cause is indeterminate, but several cases are acquainted with asthma and allergies. Some researchers believe that these nasal polyps can be attributed to the change in the mucous membrane linked with the sinuses, whereby this mucous membrane becomes inflammatory over some time and persistent, leading to fluid build-up and redness.
Nasal polyps may also be acquainted with the immune system and chemical markers in the mucous membrane.
The inflammation tends to result in fluid accumulation in the space surrounded by the mucous-forming cells known as the interstitial space. Gravitational action affects the cells by pulling them down, causing polyps.
The presence of an infection, fungi, or bacteria can cause the development of inflammation. These polyps occur mostly close to the openings of the nostrils and areas close to the nose, eyes, or cheekbones.
What are the risk factors for nasal polyps?
Any trigger of swelling or irritation in the nasal opening or cavity may lead to the growth of polyps. This can be prompted by certain conditions, which are:
- Sensitivity to aspirin.
- Inflammation and narrowing of the air passage, known as asthma
- A genetic disorder causing the formation of thick mucus in the nasal is known as cystic fibrosis.
- Deficiency of vitamin D in the body.
- Allergies to fungi that are airborne
- Eosinophilic granulomatosis with polyangiitis (EGPA) or the Churg-Strauss syndrome causing inflammation of the vessels in the blood may lead to nasal polyps.
- Hereditary can also play a part in genetic variations acquainted with the immune system.
Symptoms
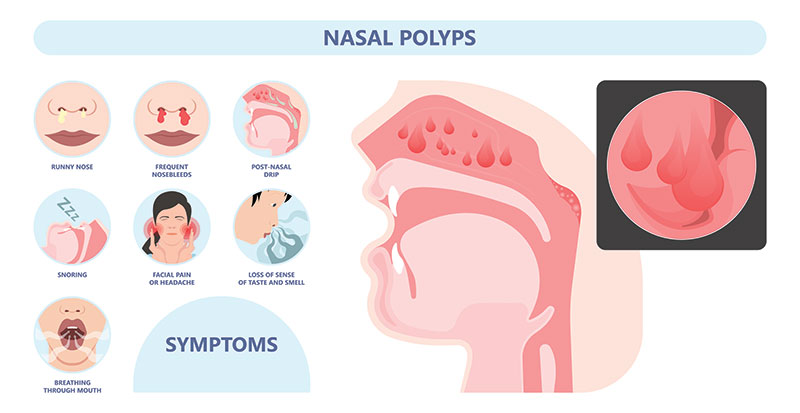
The common signs are inflammation and irritation of the airway passages. After 12 weeks of inflammation, the case is regarded as chronic sinusitis.
Signs and symptoms associated with nasal polyps are:
- Loss of sense of smell.
- Loss of sense of taste.
- Headache.
- Pains on the face.
- Postnasal dripping.
- Regular stuffiness.
- Running nose.
- Frequent snoring when sleeping.
- Bleeding from the nose.
- Pain in the teeth.
How is nasal polyp diagnosed?
Diagnosis can be made on symptoms experienced by the patient along with a general examination of the nose where a lighted material can be used to view the nose. Other diagnostic processes include:
- Imaging Studies
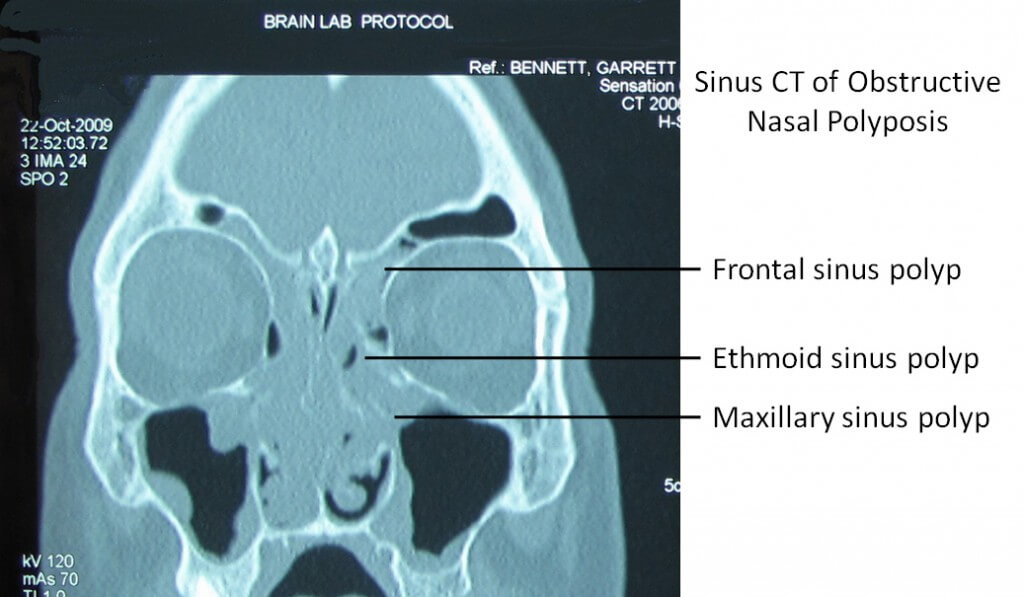
Computed tomography (CT) scan is used here to get an image of the internal structure to determine the location and size of the polyps and have a clear image of the extent of the inflammation.
- Nasal Endoscopy
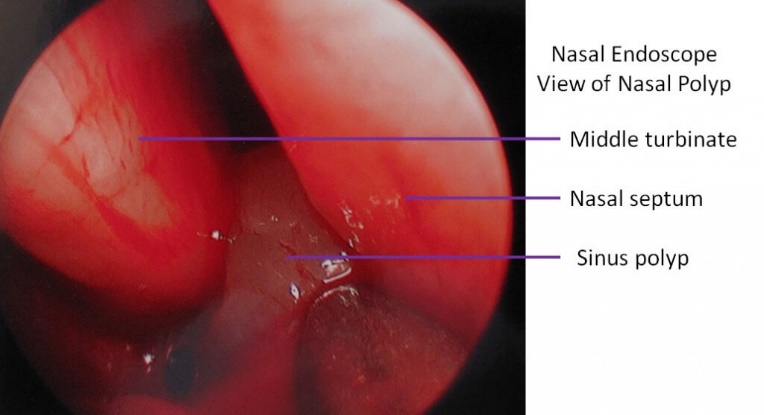
A tube, the size of a pen with a tiny camera attached to the end, is inserted into the nose, and the physical examination is done by the doctor monitoring the output of the camera on a screen.
- Allergy Tests
Skin tests might be done to check for any allergies that could lead to chronic irritation or inflammation.
- Cystic Fibrosis
Test for cystic fibrosis is done for children based on hereditary immune system defects affecting the mucus or saliva. A non-invasive sweat test is done, and the salt content deducts the presence of polyps or not.
- Blood Test
A blood test is done to determine the level of vitamin D, and the low quantity of vitamin D in the body dictates nasal polyps.
How can nasal polyps be treated?
Nasal polyps can be treated with medications or surgical procedures.
Medications The medications that can be used are:
- Nasal corticosteroids like fluticasone, budesonide e.t.c.
- Oral and injectable corticosteroids like prednisone with a nasal spray, though, are taken for a few periods due to side effects.
- Dupilumab is used for both nasal polyps and chronic sinusitis.
- Antihistamine for allergies
- Antibiotics for infections.
Nasal Polyps Surgery
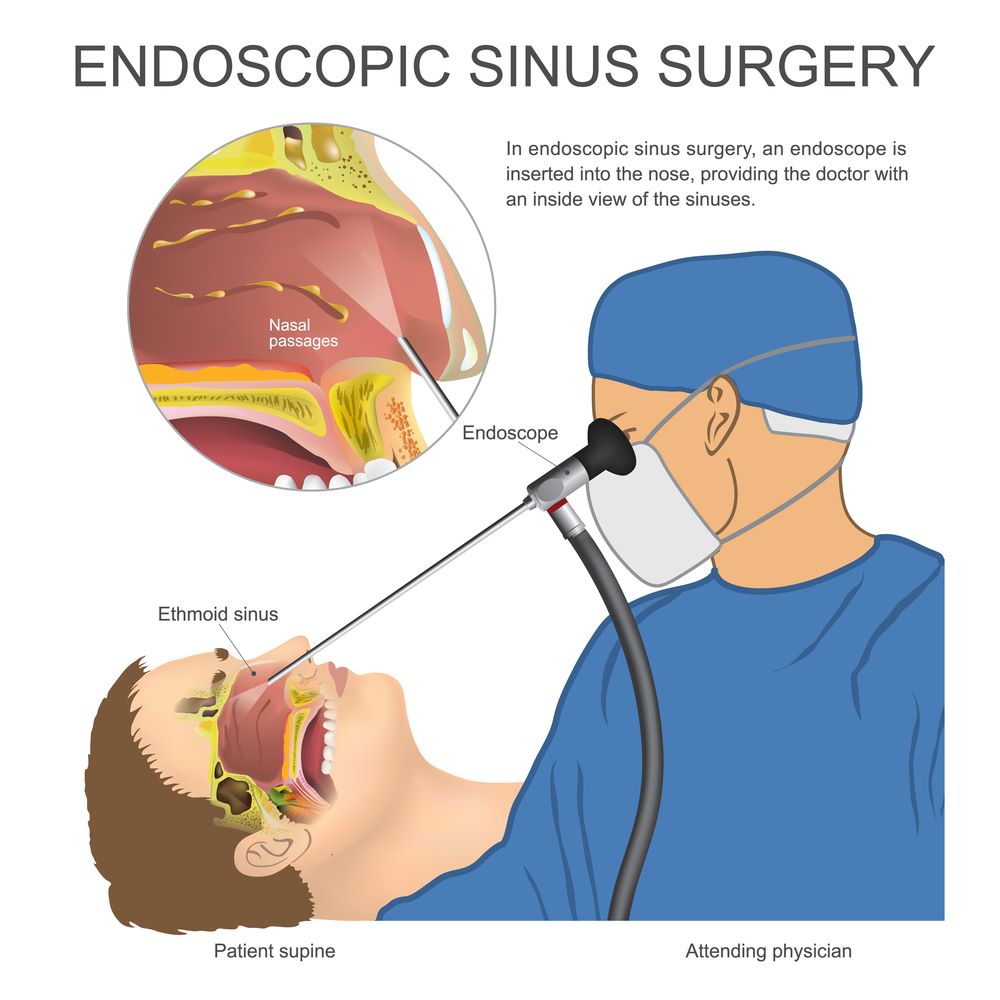
The surgical procedure is used when the medications fail to eliminate the nasal polyps. Therefore, endoscopic surgery is performed by removing the polyps and solving the sinuses problem that makes the nose liable to inflammation. Afterward, the corticosteroid nasal spray will be used to prevent recurring polyps, or a saline solution will be used.
What are the complications of nasal polyps?
Nasal polyps complicate the nasal cavity greatly as it does not permit for free flow of air into and out of the system. It also restricts fluid drainage due to the inflammation of the lining of the tissues in the nose and irritation, which happens to be long-term. These few complications as a result of the nasal polyps are explained below:
- Asthma Flare-Ups
Asthmatic patients are susceptible to nasal polyps, but equally, when the condition is severe, it can lead to flare up and aggravate asthma.
- Obstructive Sleep Apnea
This condition is a severe one as it involves obstruction of the breathing capacity of a patient. The patient tends to breathe and stops at different intervals while sleeping.
- Sinus Infection
The presence of polyps can prompt the development of certain infections caused by bacteria or fungi in the sinuses.
How can nasal polyps be prevented?
Nasal polyps can be prevented mostly after treatment of the patient due to their recurring nature. The following strategies can be used to prevent the further development of the polyps:
- Avoid Irritation of the Nasal Cavity
It is strictly recommended that airborne and toxic substances that can agitate inflammation or irritation should not be inhaled. These airborne toxic substances can be tobacco smoke, dust, debris, allergens, and chemical fumes.
- Proper Management of Allergies and Asthma
Strict adherence to prescriptions recommended by the doctor and following proper treatment plans alongside monitoring when the patient is not responding positively to the treatments administered.
- Utilization of a Nasal Rinse
Regular usage of saline water spray or wash to cleanse the passageway of the nose is beneficial and can prevent the formation of polyps as it can enhance the flow of mucus and exterminate irritants and allergens.
- The practice of Healthy Hygiene
Washing hands frequently and thoroughly is considered the best way of maintaining personal hygiene and preventing the infestation of bacteria and viruses that may lead to swelling and irritation.
- Humidification of the Environment
Humidifiers can aid in moisturizing the airway passage and influence the mucus flow from the nasal cavity. Also, they prevent inflammation and blockages.
FAQ
Yes, nasal polyps are a persistent condition, so it comes back most times after treatment. Saline solution or corticosteroid spray can be used to resist the reoccurrence of the condition.
Nasal polyps, most of the time, mimic cold, and it does not clear up easily like the actual cold itself.
Generally, nasal polyps are painless. The patient does not bleed, and it does not burst, except for cases where there is an underlying condition like sinus cancer.
When they go untreated for an extended period, pressure in the lining of the tissues can result in the expansion of the nose and the eye space.
Nasal polyps occur in all age ranges, but it is persistent in adulthood of age range between 30 to 40 years of age. Also, patients with asthma and cystic fibrosis are susceptible to the condition.
They usually occur on both sides. Nasal polyps occurring on one side may actually be something else, such as a cancerous tumor [1].
There is a possibility that nasal polyps can cause blockage in the Eustachian tube, which results in causing an increase of negative pressure in the ear which in turn causes tinnitus, dizziness, and vertigo (head spinning sensation) [2].
Treating nasal polyps early will result in a good prognosis for the patient. If left untreated, it will result in causing blockage of the nasal passage and causing breathing difficulty, recurrent infection, and loss of sensation of smell for the patient.
References
- https://my.clevelandclinic.org/health/diseases/15250-nasal-polyps
- https://mwent.net/nasal-polyps-dizziness-whats-the-connection/#:~:text=When%20a%20polyp%20forms%20in,vertigo%20(a%20spinning%20sensation).






























































































